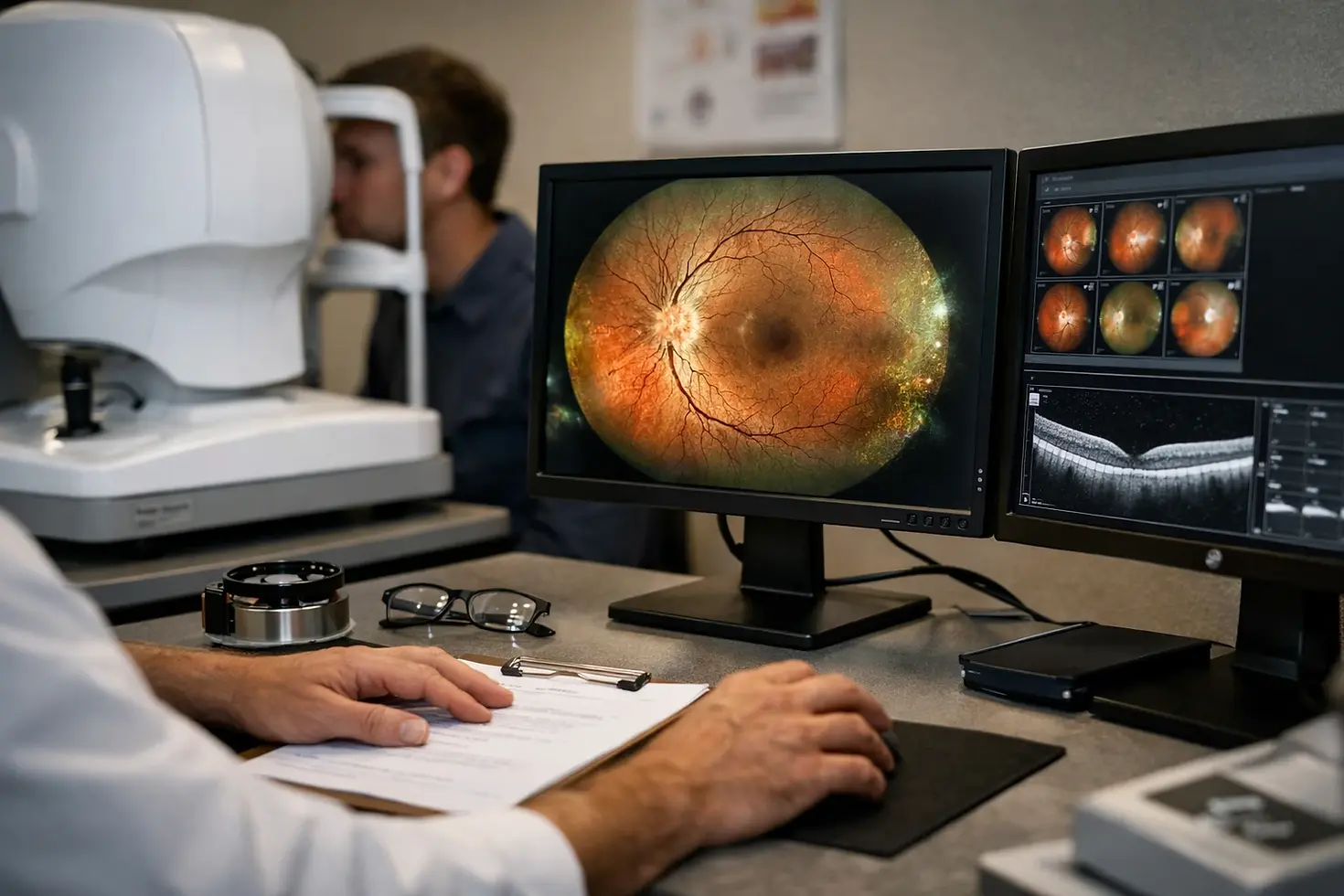
What is ultra-widefield retinal imaging
- 3 days ago
- 11 min read
At 7:40 on a winter morning, a patient from a regional town sits in a dim exam room, keeps their chin steady on the rest, and stares at one fixed target while a camera captures the back of the eye in a single, wide view. The moment is brief. The stakes are not.
That small scene explains why ultra-widefield retinal imaging matters. You are not looking at a routine photograph. You are looking at a way to document much more of the retina — including the far edges, where disease can sit quietly — without turning a long appointment into an ordeal. If you are dealing with diabetes, retinal tears, inflammation, macular disease, glaucoma, or even cataract planning where retinal status matters, this topic is worth understanding.
This page is for patients, carers, and referring clinicians who want a practical explanation of what ultra-widefield retinal imaging does and how different options should be weighed. If you are travelling from Dubbo, Orange, Wagga Wagga, Canberra, Liverpool, Randwick, or the Hills district for specialist eye care, the first imaging session often needs to count.
Selection criteria: what to compare before you choose an ultra-widefield retinal imaging option
How much retina the system can capture
Start with coverage. EyeWiki describes retinal imaging as the creation of a two-dimensional image of three-dimensional retinal tissue and calls it indispensable for diagnosis and management in ophthalmic practice. That is the baseline. The real question is how much of the retina can be seen in a usable image, especially when you are worried about disease outside the central view.
Wide-field and ultra-widefield systems are used across a broad clinical range: diabetic retinopathy, hypertensive retinopathy, age-related macular degeneration, vascular occlusions, vasculitis, retinal detachment, glaucoma, systemic infections, leukemias, and systemic malignancies with ocular metastasis are all listed by EyeWiki as relevant applications. Several instruments are available today. That means the better choice is not the one with the loudest marketing. It is the one that gives your clinical team the retinal map they actually need.
If the disease can hide in the periphery, the selection criteria should start with field of view, not brand.
How quickly it captures usable images
Speed sounds like a convenience feature until you sit in the chair yourself. A patient with neck stiffness, tremor, fatigue, photophobia, poor fixation, or anxiety does better when the image is obtained quickly and cleanly. So does a busy clinic in Canberra or Liverpool that needs reliable imaging before dilation wears off or the waiting room fills.
Fast capture also reduces repeat positioning. That matters in older adults, in children, and in patients who have already travelled several hours for review. A technician reviewing the scan beside you wants a usable image on the screen, not a half-complete set that has to be repeated three times.
Whether it supports diagnosis, follow-up, and case review
A broad image is only useful if it can be compared over time, reviewed alongside symptoms, and shared for referral or second opinion. Imaging should support three jobs: diagnosis at the first visit, follow-up at the next visit, and case review when management changes. If the system makes those steps clumsy, the field of view alone will not save it.
For patients from rural and regional communities, this point is easy to underestimate. If your first scan is clear, shareable, and easy to review later, the next decision may be faster and more confident.
#1 Single-shot ultra-widefield cameras
Summary: These systems aim to capture a very broad retinal view in one fast image, with minimal repositioning.
Best for: Clinics that want broad retinal coverage with as little repositioning as possible, especially for screening, triage, and high-throughput review.
What single-shot capture means
Single-shot capture means that the machine is designed to document a very wide area of the retina in one image rather than building the record from multiple smaller images. One major manufacturer describes its platform as producing a 200-degree single-shot ultra-widefield retinal image. That figure is often cited because it signals breadth, speed, and practicality in a single line.
For you as a patient, the plain-language meaning is simple: look at one target, keep still, and the system captures far more peripheral retina than a standard central photo. It is not magic, and it does not remove every limitation — lashes, lids, media opacity, and patient movement still matter — but it can change how much is visible in a short appointment.
Why it helps in busy or hard-to-image patients
One fast capture can be easier on patients who struggle with repeated positioning, long visits, or limited stamina. I have seen this make a real difference in people with back pain, Parkinsonian tremor, poor mobility, and those who are simply exhausted after travel. Shorter imaging is not a luxury. It is often what makes imaging possible at all.
One fast capture can be easier on patients who struggle with repeated positioning, long visits, or limited stamina.
In a regional referral pathway, that matters twice. It improves patient experience on the day, and it increases the chance that the specialist receives something useful rather than a partial set.
Where it fits in a referral or screening workflow
Single-shot systems fit well at the front end of care: baseline documentation, diabetic eye screening, urgent triage, and referral workups. They also suit follow-up visits where the main question is whether the peripheral retina looks stable or newly active.
Some platforms extend that value with interpretation support. A widely used manufacturer describes a searchable pathology resource built from recent ultra-widefield retinal images and OCT scans, organised by pathology and image modality. That kind of structure can help clinicians compare what they are seeing on screen with known patterns — especially when the concern sits in the periphery rather than the macula.
#2 Wide-field retinal imaging systems for complex diagnosis and management
Summary: These systems are built for documentation across a broad range of retinal and vascular conditions, not just quick capture.
Best for: Eye care teams that need wide documentation to support diagnosis, treatment planning, and long-term follow-up in complex disease.
Conditions where wide-field documentation matters
Complex diagnosis starts with seeing enough. EyeWiki notes that retinal imaging helps practitioners directly view retinal disease and plan treatment according to the pathology. That sounds obvious, but it becomes far more powerful when the disease does not sit in the centre of the retina.
The list of relevant conditions is long and clinically serious: diabetic retinopathy, hypertensive retinopathy, age-related macular degeneration, vascular occlusions, vasculitis, retinal detachments, glaucoma, systemic infections, leukemias, and systemic malignancies with ocular metastasis. When those possibilities are on the table, wider documentation is not about collecting prettier images. It is about not missing what matters.
Why the peripheral retina changes management
The peripheral retina can change the plan. A lesion at the edge may shift the decision from observation to closer monitoring, from routine referral to urgent review, or from one treatment pathway to another. This is why clinicians who manage retinal disease often speak about peripheral findings with real respect.
Wide-field imaging is not just about taking a bigger photo; it can change what gets treated, monitored, or referred.
Picture a follow-up visit with peripheral lesions visible on a large monitor. That image can influence whether the next step is review, procedure, laser, medical treatment, or transfer of care. A narrow central image cannot do that job if the decisive change is off to the side.
How wide-field imaging supports treatment planning
Wide-field and ultra-widefield systems sit within the broader evolution of modern digital retinal imaging. That point from EyeWiki matters because these systems are not isolated gadgets. They are part of how treatment planning, documentation, and communication now happen in retina care.
If you are travelling from a regional area into a specialist clinic, strong documentation can shorten the gap between imaging and a management plan. If you are preparing for cataract surgery and your doctor needs to confirm that the retina is stable first, good wide-field imaging can also make that conversation sharper and more useful.
#3 Multimodal imaging workflows
Summary: These workflows combine a wide retinal photograph with another imaging method so the clinician can answer more than one question in the same visit.
Best for: Practices that want one imaging session to inform diagnosis, confirmation, and follow-up without making the process confusing for staff or patients.
Pairing ultra-widefield images with OCT
Ultra-widefield imaging gives you the map. OCT gives you the slice. Put plainly, a wide retinal image shows the layout across the retina, while OCT shows a cross-sectional view of retinal layers in detail. When both are reviewed together, central structure and peripheral findings can be interpreted in context rather than in isolation.
EyeWiki includes multimodal imaging as part of the conversation around wide-field and ultra-widefield systems. That reflects routine clinical reality. A suspicious haemorrhage, pigment change, or area of traction may need a second view before you decide what it means.
Using multimodal review for confirmation
A wide-field image is stronger when it can be reviewed alongside another modality instead of standing alone. One manufacturer’s pathology reference is built specifically around this principle, helping clinicians identify patterns in both ultra-widefield retinal images and OCT scans, searchable by pathology and by image type.
A wide-field image is stronger when it can be reviewed alongside another modality instead of standing alone.
This is especially useful when the first image raises, rather than resolves, the clinical question. The widest view in the world still benefits from confirmation when treatment decisions are being made.
Keeping the workflow manageable for staff and patients
Multimodal does not need to mean cumbersome. The best workflows are the ones staff can repeat reliably: clear sequencing, predictable file review, and easy comparison on two side-by-side screens. If a clinician can look at the wide image and the OCT during the same discussion, the appointment becomes more efficient and easier for you to follow.
That matters in mixed clinics, where retinal disease, cataract assessment, and urgent add-on patients can all appear in the same half day. Good imaging should reduce friction, not create it.
#4 Technology comparison resources for choosing among multiple systems
Summary: Comparison-focused resources help you make sense of several available imaging technologies without reducing the decision to a single specification.
Best for: Clinics evaluating more than one platform, or patients who want to ask smarter questions about how their imaging will be done.
What a comparison-focused article can help with
The practical problem is simple: several instruments are available today, and many promise broad imaging. A 2023 continuing education article, Ultra-Widefield Imaging: Expand Your Horizons, credited to Julie Torbit, OD, and Brad Sutton, OD, is framed around that exact issue — helping clinicians work through technologies to obtain optimal results for many common retinal conditions.
That framing is useful because it puts the emphasis where it belongs: not on novelty, but on outcomes. You do not need the newest console in the room. You need the imaging approach that answers the questions your clinic sees every day.
How to define 'optimal results' for your practice
Optimal results depend on case mix. A clinic seeing large volumes of diabetic retinopathy and vascular disease may prioritise peripheral documentation and repeatable follow-up. A practice serving older cataract patients may care deeply about speed, comfort, and whether retinal status can be documented efficiently before surgery. A tertiary referral service may value image review and sharing above all else.
Buy for the patients you see most often, not the feature you are least likely to use.
That same advice helps patients. When you ask about imaging, ask how it helps with your condition, not how many features sit on the brochure.
Questions to ask before you commit
If you are choosing a clinic or helping to choose a system, ask direct questions. How much retina can be captured in one visit? How quickly can a usable image be obtained? Can the image be reviewed alongside OCT or prior scans? Is it easy to share for second opinion or specialist referral?
Those questions often tell you more than a product name will. They also keep the discussion anchored to patient care, where it belongs.
#5 Pathology libraries and interpretation support
Summary: Searchable case libraries help clinicians compare retinal findings against organised examples and support more consistent interpretation.
Best for: Teams that want to improve reading confidence, train newer staff, and support remote or second-opinion review.
Searchable examples by pathology
Interpretation support is often overlooked when clinics discuss imaging. Yet it can be one of the most useful features around the machine. A well-known pathology reference in this space is described as a searchable decision-support tool, with case images from recent ultra-widefield technology organised by pathology and image modality.
That structure matters because retinal disease does not present as tidy textbook boxes in real clinics. Searchable examples help a clinician move quickly from “this looks unusual” to “this pattern resembles a known entity that needs closer review.”
Using image libraries for training
An image library does not replace clinical judgment, but it can shorten the learning curve for peripheral lesions. That is valuable in teaching settings and in practices where technicians, orthoptists, optometrists, and ophthalmologists all interact with the imaging pathway.
An image library does not replace clinical judgment, but it can shorten the learning curve for peripheral lesions.
Picture a senior clinician pointing to a desktop monitor during a teaching session, comparing one retinal image against a curated set of similar cases. That is not marketing theatre. It is how pattern recognition is built responsibly.
Supporting remote or second-opinion review
For rural and regional networks, interpretation support has a second role: it strengthens communication. A clear image, matched against a known pattern and sent with a concise note, makes second-opinion review more efficient. That can help when the first clinic is hours away from the retinal surgeon or tertiary centre.
If you have ever made a long trip only to hear that more information is needed before a decision can be made, you already understand why this matters.
How to choose the right ultra-widefield retinal imaging option
Match field of view to the diseases you need to document
Ultra-widefield imaging is used to help view and manage a wide range of ocular and systemic conditions, not just one disease category. So the first question is clinical, not technical: what are you trying to see? If diabetic retinopathy, vasculitis, vascular occlusion, retinal breaks, or peripheral degeneration sit high on your list, broader field of view should carry more weight.
If your main need is central macular assessment, wide imaging may still matter, but it may need to sit within a broader multimodal workflow rather than act alone. Match the view to the pathology you expect, not the headline claim on the device sheet.
Match capture speed to patient comfort and clinic flow
A 200-degree single-shot capability is attractive because it speaks directly to workflow and comfort. That kind of speed can reduce repeat positioning, help staff obtain images in difficult circumstances, and make the visit easier for patients with limited stamina or long travel days.
For clinics serving regional NSW or the ACT, speed has strategic value. The faster a high-quality image can be obtained, the more likely it is that the first appointment delivers enough information for a treatment plan or a decisive referral. For patients travelling into Canberra, Liverpool, Randwick, or the Hills district to see a specialist such as Dr Rahul Dubey, that is not a minor convenience. It can shape whether the next step happens now or weeks later.
For rural and regional patients, the best option is often the one that reduces repeat visits and makes the first visit count.
Match interpretation support to your experience and referral pathway
If the team reading the images is highly experienced, interpretation support may be a welcome extra. If the team is mixed, growing, or working across distance, it may be essential. Searchable case libraries, organised by pathology or image type, can improve consistency and support cleaner referrals.
You should also think beyond the image itself. Can it be reviewed with OCT? Can it be compared easily over time? Can it be shared for specialist opinion without friction? Those questions usually determine whether imaging becomes a genuine clinical asset or just another file on a server.
Ultra-widefield retinal imaging gives you a broader, more actionable view of the retina when timing, travel, and diagnostic accuracy all matter.
If you are balancing retinal disease, cataract planning, or long travel from a regional town, the right imaging setup can make the first visit more useful and the follow-up more precise. When you next discuss ultra-widefield retinal imaging, which matters most to you — wider coverage, quicker capture, or stronger specialist review?




Comments