Complete Guide to Optomap Retinal Imaging
- 15 hours ago
- 10 min read
Table of Contents
A patient sits in a dim exam room. A technician asks them to rest their chin, keep both eyes open, and look toward a small green target. A second later, a panoramic image of the back of the eye appears on the monitor. The room stays quiet for a beat. Then the questions start.
That scan is optomap retinal imaging, a quick ultra-widefield view of the retina — the light-sensitive tissue lining the back of your eye. It matters because a larger image can change what your clinician sees in one visit, what gets documented for later review, and how easily your care can be coordinated if your eye health is complicated.
If you live with diabetes, glaucoma risk, macular disease, cataracts, or several eye issues at once, that wider view is practical, not theoretical. For patients travelling between a local optometrist and a specialist clinic in Canberra, Liverpool, Randwick, or the Hills district, I have seen one clear retinal image save an extra trip and sharpen the next decision.
Fundamentals of Optomap Retinal Imaging
What optomap retinal imaging captures
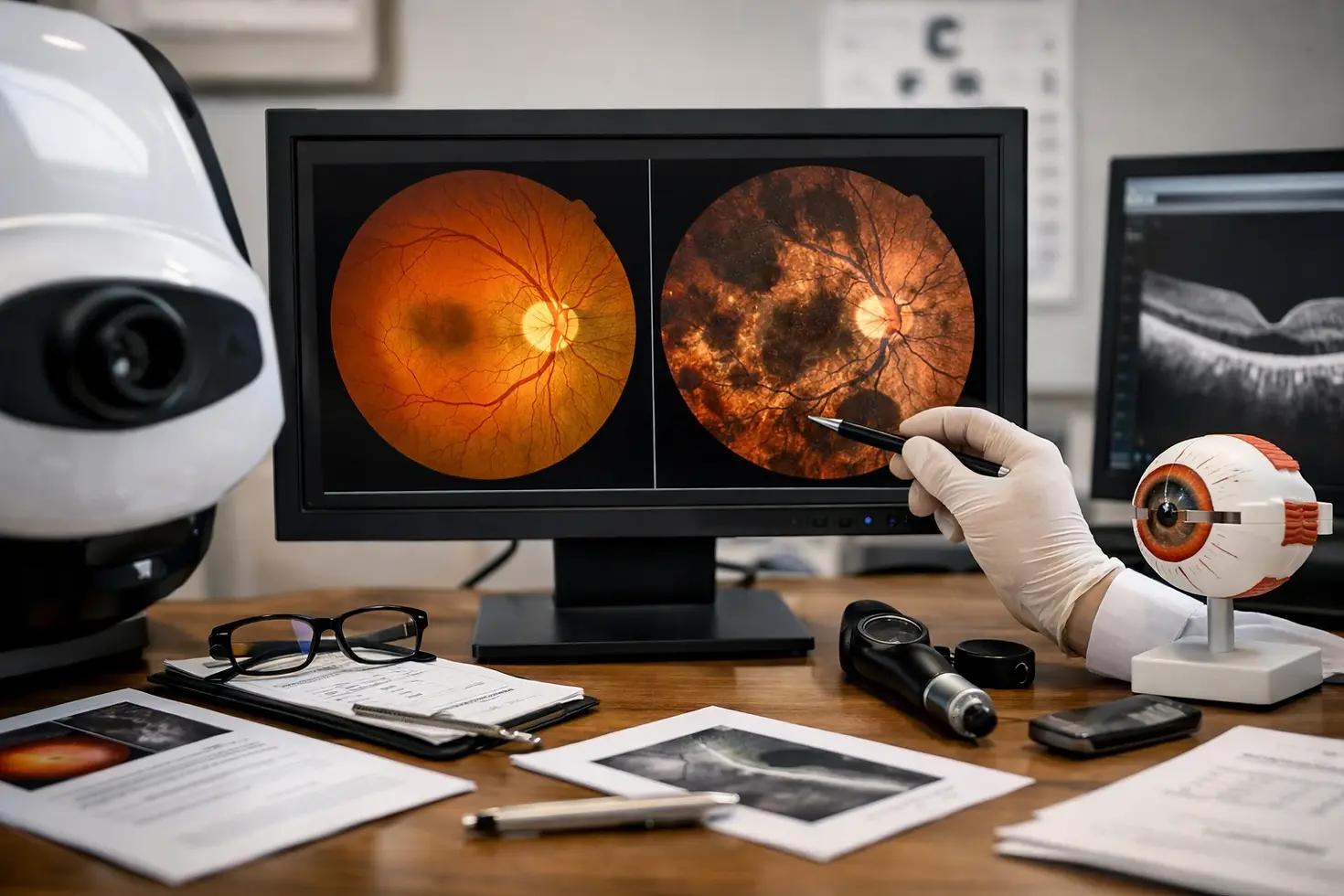
Optomap retinal imaging captures a very wide image of the retina in a single scan. That includes the central area used for detailed vision, the optic nerve, the retinal blood vessels, and much of the outer retina that standard photographs may miss. In plain language, you are not just getting a close-up of the middle. You are getting a broad map.
That distinction matters. Traditional small-field and even widefield retinal imaging may capture only 10 to 100 degrees of the retina in a single image. By contrast, optomap is described as a clinically validated ultra-widefield image that can capture 200 degrees, or about 82% of the retina, in one shot. With auto-montage, using multiple captures stitched together, that can extend to 220 degrees, or up to 97% of the retina.
Why a wider retinal view matters for complex eye care
A wider field changes the conversation because disease does not always stay neatly in the centre of the retina. Some findings sit near the periphery, away from the area you use to read or recognise faces. If the image only shows the middle, the record is limited from the start.
A wider retinal view is valuable because it can show the central pole, mid-periphery, and periphery in one exam.
The central pole is the middle back part of the eye, including the macula and optic nerve. The mid-periphery and periphery are the outer regions. When you can see all three together, clinicians can spot patterns, compare changes over time, and explain your condition more clearly. That is especially useful if you have multiple risks at once — for example, diabetes plus cataract, or glaucoma surveillance plus a family history of retinal disease.
Which eye conditions it helps monitor
Top clinical pages consistently describe this technology as useful for detecting and monitoring conditions such as diabetic retinopathy, age-related macular degeneration, and glaucoma. The reason is straightforward: these conditions can affect the retina, optic nerve, and blood vessels in ways that become easier to document when the field of view is broad.
Diabetic retinopathy: bleeding, leakage, and other retinal changes may be documented and tracked over time.
Age-related macular degeneration: changes near the macula can be reviewed alongside the wider retinal background.
Glaucoma: the optic nerve appearance can be recorded as part of a larger eye assessment.
General retinal monitoring: a broader baseline helps when new symptoms or referral questions arise later.
This does not mean one scan answers everything. It means you start with a better map.
How Optomap Retinal Imaging Works
What the technician does during the scan
The mechanics are simple. You sit at the instrument, place your chin and forehead in position, and look at a target. The technician adjusts your alignment, asks you to keep still, and captures the image. Usually, each eye is scanned separately. Sometimes a repeat image is taken if a blink, lashes, or dry eye has reduced clarity.
The system is described as non-invasive and capable of capturing a 200-degree digital image in a single scan. Unlike conventional devices that use full-spectrum white light, optomap technology uses low-powered laser wavelengths that scan simultaneously. For most patients, the experience is brief. You are not touched by the machine. You simply hold steady for a moment.
The scan is designed to be quick and non-invasive, which helps make retinal imaging easier to complete during a routine visit.
Why dilation is not always required
One reason many clinics offer this scan routinely is that dilation is not always required. In many cases, the image can be captured through an undilated pupil. That can make the visit easier if you need to drive, return to work, or bring a family member to the appointment.
Still, you should not hear “often no dilation” as “never dilation.” If your pupils are small, if media clarity is reduced, if cataract is affecting the view, or if symptoms suggest a problem that needs a closer examination, dilating drops may still be recommended. A careful clinician does not skip a needed exam step just because a wide image was obtained first.
What the image shows clinicians after capture
Once the image is captured, your clinician reviews a large retinal photograph that can show the optic nerve, macula, blood vessels, and broad peripheral retina in the same record. That matters for both diagnosis and documentation. In clinic, we often compare the current image with prior scans to answer a simple question: what has changed since the last visit?
That side-by-side review is where the technology becomes more than a picture. It becomes a timeline. For a patient with diabetes over 5 or 10 years, for example, a saved image can show whether retinal findings are stable, improving, or developing in a way that needs treatment or referral.
Best Practices for Getting the Most From Optomap Imaging
Before the appointment
Annual eye exams remain vital for vision and general health, and imaging works best when it sits inside that larger visit. Before your appointment, bring a short symptom history, a current medication list, and details about medical conditions such as diabetes or hypertension. If you already have eye records from another practice, bring those too. That is particularly helpful if you live in a rural or regional area and your care is split across sites.
Your retina is the only place in the body where blood vessels can be seen directly. That is why retinal findings can sometimes reflect broader health issues. Early signs linked to stroke, heart disease, hypertension, and diabetes may appear in the retina before you notice a change in vision. If your blood sugar has been unstable, or your blood pressure has been difficult to control, say so. The scan is better interpreted in context.
During the imaging session
Good image quality depends on a few small things. Sit comfortably. Blink just before the technician tells you to hold still. Keep your forehead firm against the bar. If you are sensitive to light, have a very dry eye, or are seeing a large floater that keeps crossing your vision, mention it before the first capture. A 20-second conversation can prevent a poor-quality record.
Tell the technician if you have had recent flashes, new floaters, blur, or distortion.
Let them know if you struggle to hold one eye steady.
Expect a repeat image if lashes, blinking, or tearing obscures part of the scan.
Ask whether the scan will be compared with previous images from last year or from another clinic.
Best practice is to treat the image as part of the conversation, not the whole diagnosis: the scan supports clinical judgment, it does not replace it.
After you receive the image report
This is where many patients lose value. They have the scan done, hear “looks fine,” and leave. Ask for more. Ask what the clinician is looking at, whether anything needs watching, and when the next image should be taken. If a finding is present, ask whether it is stable, suspicious, or urgent.
Three questions work well:
What looks normal on my scan?
Is there anything that needs follow-up, and on what timeline?
Should I keep a copy of this image for future comparison or referral?
If your care involves several providers, keep your report. For a patient travelling from a regional town into Canberra for specialist review, a saved retinal image can turn a vague history into a precise handover.
Common Mistakes
Assuming the scan replaces every other exam
This is the most common misunderstanding. Optomap imaging is valuable, but it is one tool within comprehensive eye care. The strongest clinical pages describe it as part of an eye exam, not a replacement for every other assessment. You may still need vision testing, eye pressure measurement, slit-lamp examination, optical coherence tomography, visual fields, or dilated fundus examination depending on the problem.
The broader value of the technology is often tied to diagnosis, treatment planning, and patient engagement. Published material around the platform refers to more than 2,500 published and ongoing clinical trials, along with thousands of case studies and testimonials. That supports serious clinical use. It does not turn one scan into a complete answer.
Missing follow-up when symptoms change
A normal image from last month does not protect you from a new problem today. If you develop sudden floaters, flashes, a curtain over part of your vision, abrupt blur, or significant pain, you need prompt review. Do not wait for your next routine imaging appointment simply because your last scan was reassuring.
I have seen this mistake more than once. A patient keeps a clean image report from March, develops new symptoms in June, and assumes nothing serious can have changed. Eyes do not work that way. Symptoms always outrank old reassurance.
Thinking a normal image rules out all disease
The retina can reflect systemic disease, but a normal-looking image does not rule out every eye condition or every medical problem. It also does not remove the need for medical follow-up if your risk factors remain high. If you have diabetes, vascular risk, strong family history, or ongoing symptoms, the right next step may still be further testing or review.
Do not confuse “widefield” with “complete” — a retinal image helps reveal more, but it does not answer every question by itself.
Tools and Resources: Where Optomap Fits in a Larger Care Plan
What clinicians can document with ultra-widefield imaging
Optomap is presented as an integrated hardware and software platform, and that matters because documentation is not just about taking a picture. It is about storing, comparing, annotating, and sharing a consistent record. Clinicians can document findings across the central pole, mid-periphery, and periphery in one system, then use that record during follow-up or referral.
For you, the practical benefit is clarity. A documented image can support referrals, second opinions, and treatment planning far better than a memory of what was said in the room. If an abnormal area is being watched, the exact location can be reviewed later rather than described vaguely as “something near the edge.”
How it supports monitoring over time
Monitoring is where ultra-widefield imaging earns long-term value. A stable image one year and a changed image the next tell a very different story than a single isolated scan. That is why follow-up intervals matter. Six months, 12 months, or sooner — the schedule depends on your risk and findings, but the principle is the same: comparison drives better decisions.
This also improves patient engagement. When you can see the same area on two visits and understand what has changed, discussions become more concrete. That is one reason the platform is frequently described as useful not just for diagnosis, but for treatment planning and patient engagement as well.
How rural and regional patients can use it in care planning
Patients outside major centres often carry the heaviest coordination burden. You may see a local optometrist, a general practitioner who manages diabetes or blood pressure, and then travel to a specialist clinic for retinal or cataract care. In that setting, a clear image record is not a convenience. It is infrastructure.
For patients in rural or regional communities, a clear image record can make referrals and follow-up planning more efficient.
If you are travelling from regional New South Wales or the ACT into the Hills district, Canberra, Liverpool, or Randwick, ask for a copy of your imaging report and the date it was taken. That simple step can reduce repeated explanations, shorten triage, and help the next clinician decide whether you need routine review, closer monitoring, or urgent treatment.
When Optomap Is Especially Useful for Complex Eye Care Needs
Retinal disease monitoring
This scan is especially useful when retinal disease risk is already on the table. If you have diabetic retinopathy, age-related macular degeneration, glaucoma surveillance, or unexplained retinal findings that need watching, a panoramic 200-degree image provides a strong baseline. You can return to the same record later and ask a disciplined question: is the picture stable or not?
That matters because complex eye care rarely depends on one appointment. It depends on trends. A broad image today may guide the timing of your next review, whether additional testing is needed, or whether the pattern supports referral for more specialised care.
Coordinating care across providers
Many patients do not receive all eye care in one room. Your optometrist may first detect the problem. Your GP may be managing diabetes, heart disease, or hypertension. An ophthalmologist may then assess whether treatment or surgery is needed. When the retina can show clues linked to systemic disease as well as eye disease, a shared image becomes a common reference point for all three.
If you are referred for further review, bring the report. That applies whether the next visit is local or whether you are travelling across Sydney, Canberra, or from a rural town to a metropolitan clinic. A good image does not replace a referral letter, but it often makes the referral more specific and the first specialist visit more productive.
When a broader retinal view adds value
The broader view adds the most value when your eye care is already complex: several diagnoses, uncertain symptoms, long travel distances, or multiple clinicians involved at different times. It is also helpful when treatment decisions depend on a reliable baseline rather than a one-line description in a file.
If your eye care is complex, the main value is not just the picture itself — it is the clearer baseline it gives your care team.
That is why patients with retinal concerns, cataracts, or hard-to-coordinate care often benefit from asking not only, “Should I have the scan?” but also, “How will this image be used over time?” In a specialist setting, including practices such as Dr Rahul Dubey’s, the answer should connect directly to monitoring, referral planning, and treatment decisions rather than marketing language.
Optomap retinal imaging gives you a faster, broader look at the retina — and that wider record can sharpen monitoring, referrals, and decisions when eye care becomes complicated.
It works best when you treat it as one part of a full assessment, ask for the findings in plain English, and keep your images available for future reviews.
If you are balancing retinal risk, cataract planning, or travel from a regional area, what might change if your care team could compare the same image over time?




Comments