
What is the difference between optometrist and ophthalmologist
- 1 day ago
- 9 min read
Table of Contents
It is 8:10 a.m. in a rural clinic. A patient with cloudy vision in one eye and a burst of new floaters in the other is trying to decide whether this is a routine eye check or something more serious. They are not looking for theory. They want the right door, fast.
If you have ever typed “what is a ophthalmologist” into your phone after a worrying change in vision, the short answer is simple: optometrists usually handle routine vision care, while ophthalmologists are medical eye doctors who diagnose eye disease, prescribe treatment, and perform surgery when needed. That difference matters most when cataracts, glaucoma, diabetic eye disease, macular degeneration, flashes, floaters, or sudden vision loss enter the picture.
What is a ophthalmologist, exactly?
An ophthalmologist is a medical eye doctor who can diagnose eye disease, treat it with medicine or procedures, and operate when your sight is at risk.
A doctor for eyes and vision
You should think of an ophthalmologist as the specialist for the full medical side of eye care. That includes examining the eye, identifying disease, prescribing medication, recommending glasses or contact lenses when helpful, and deciding whether a procedure or operation is needed.
This is the clinician you see when the problem goes beyond “Do I need a new prescription?” and becomes “Why is my vision getting cloudy?”, “Why am I seeing flashes?”, or “Why did my sight drop suddenly?” Cataracts, glaucoma, retinal tears, and diabetic eye disease all sit in this medical territory.
An ophthalmologist is the eye specialist you want when the problem may need medication, procedures, or surgery.
What conditions they treat
Ophthalmologists treat a broad range of conditions affecting the eyes and vision. Common examples include cataracts, glaucoma, macular degeneration, diabetic retinopathy, and retinal detachment. Many also assess floaters and flashes, eye inflammation, and other structural problems inside the eye.
The practical point is this: these are not just “vision problems.” They are medical conditions. A cataract clouds the eye’s natural lens. Glaucoma can damage the optic nerve. Diabetic retinopathy affects the retina — the light-sensitive tissue at the back of the eye. Retinal detachment is an urgent threat to sight.
What training they complete
Ophthalmologists complete medical training first and specialty training after that. In the U.S., the standard pathway described by major medical sources is a four-year undergraduate degree, medical school, a one-year internship, and at least three years of specialist medical and surgical training in eye care. The country may change; the core idea does not. This is physician-level training with surgical capability.
That background is why ophthalmologists can bring diagnosis, medicine, imaging interpretation, procedures, and surgery into one treatment pathway. When you are deciding who should assess cataracts or a retinal problem, that difference is not academic. It shapes what can be done at the first visit.
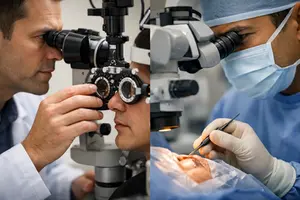
How is an ophthalmologist different from an optometrist?
The difference is straightforward: optometrists focus on routine vision care and first-line eye assessment, while ophthalmologists handle medical eye disease and surgery.
Routine eye exams and glasses versus disease treatment
Optometrists commonly perform routine eye exams, check whether you need glasses or contact lenses, and monitor many day-to-day vision issues. They are often the first professional to notice that something more serious may be happening. That role matters. Many cases of glaucoma, cataracts, and diabetic eye disease are first detected during a routine visit.
An ophthalmologist steps in when the issue becomes medical or surgical. If the answer may involve prescription medicine, injections, a laser procedure, cataract surgery, or retinal surgery, you are no longer in routine-vision territory. You are in specialist care.
Who performs surgery
Ophthalmologists perform eye surgery. Optometrists generally do not. That is the cleanest dividing line.
If you need cataract surgery, treatment for retinal detachment, surgery for a macular hole, or another operation inside or around the eye, you need an ophthalmologist. Even before surgery is discussed, the ability to decide whether surgery is needed changes how the whole consultation works.
When you may be referred
You may be referred from an optometrist to an ophthalmologist when an exam suggests cataracts, glaucoma, retinal disease, diabetic retinopathy, macular degeneration, or a sudden structural problem such as a retinal tear. That referral is not a failure of routine care. It is the right handoff.
For many patients, the smoothest path is shared care: an optometrist identifies the concern, an ophthalmologist confirms the diagnosis and treats it, and follow-up may then be coordinated locally where appropriate.
Rule of thumb: if the answer might involve medicine, imaging, or surgery, you’re in ophthalmologist territory.
Why does the difference matter for cataracts or retinal conditions?
It matters because cataracts, glaucoma, and retinal disease are not just about blurry vision — they can threaten sight if treatment is delayed or sent down the wrong pathway.
Cataracts and glaucoma often need medical management
Cataracts and glaucoma are common reasons people see an ophthalmologist. Cataracts usually cause progressive clouding, glare, and faded vision. The treatment decision is based on function: reading, driving, work, depth perception, and day-to-day safety. That decision becomes a medical and surgical judgment, not only a prescription update.
Glaucoma is even more unforgiving. You may not feel it early. You may not notice the field loss until damage has already occurred. Pressure checks, optic nerve assessment, scans, drops, laser, and sometimes surgery can all come into play. This is why a “just get new glasses” mindset can miss the real problem.
Retinal diseases need specialist evaluation
Retinal conditions sit at the sharper end of urgency. Diabetic retinopathy can damage retinal blood vessels. Macular degeneration affects central vision. A retinal tear or retinal detachment can cause flashes, floaters, or a shadow across your sight. Those problems are not corrected with a stronger lens.
If your retina is involved, time matters. A patient who lives two hours from a major centre may be tempted to wait until next week. That can be a costly decision. With new floaters, flashes, or a curtain-like shadow, you need prompt specialist assessment.
Why earlier treatment matters
Earlier treatment matters because some vision loss can become permanent. A delayed cataract review may mean months of avoidable visual disability. A delayed glaucoma diagnosis may mean silent optic nerve damage. A delayed retinal assessment can be much worse.
This is where the difference between optometrist and ophthalmologist becomes practical. If the issue could scar the retina, raise eye pressure, or require surgery, you should not stay in the routine-care lane longer than necessary.
If vision loss could be permanent, don’t keep it in the “just get new glasses” category.
How does care with an ophthalmologist work?
Care with an ophthalmologist usually moves through three steps: diagnosis, treatment planning, and follow-up under the same medical specialist.
Exam and diagnosis
The first visit starts with your story. When did the symptoms begin? Was the change sudden or gradual? Is there pain, glare, distortion, flashes, or a missing patch of vision? Your sight is then measured, the front and back of the eye are examined, and drops may be used to dilate the pupils so the retina and optic nerve can be seen properly.
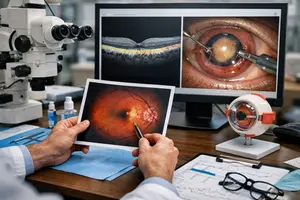
You may also need photographs or scans. For cataracts, the lens is assessed. For glaucoma, pressure and optic nerve findings are reviewed. For diabetic retinopathy or macular disease, retinal imaging helps show what is happening inside the eye. None of this is guesswork. It is a structured medical assessment.
Medication, testing, and vision aids
Not every appointment ends with surgery. Ophthalmologists can prescribe medication, order or interpret testing, and recommend glasses or contacts when they are still part of the best answer. A patient with early glaucoma may start drops. A patient with inflammation may need medicine. A patient with stable vision issues may still benefit from updated lenses.
This is often where people are surprised. They assume an ophthalmologist only operates. In reality, the specialist may manage the whole pathway — including deciding that surgery is not needed yet.
A practical rule: ophthalmologists don’t only “send you to surgery” — they can manage the whole treatment pathway.
Surgery and follow-up
When the condition does require an operation, the same specialist framework continues. Cataract surgery, retinal procedures, and other treatments are followed by review visits, medication adjustments, healing checks, and ongoing monitoring. Good care does not stop in the operating theatre.
For people dealing with complex cataracts, diabetic retinopathy, retinal detachment, or persistent floaters, that continuity matters. The same service that made the diagnosis can usually explain the risks, perform the procedure, and monitor the result over time.
When should you see an ophthalmologist urgently?
You should seek urgent eye assessment when symptoms begin suddenly, worsen quickly, or suggest a retinal, pressure-related, or inflammatory problem.
New flashes or floaters
New flashes or floaters should be treated as urgent, especially if they arrive in a shower, come with a shadow, or are followed by a curtain-like loss of side vision. An ophthalmology service commonly evaluates floaters and flashes because they can signal a retinal tear or detachment.
One floater you have had for years is different from twenty new ones today. That distinction matters. So does timing. Same day is the safest frame of mind.
Sudden pain, redness, or vision loss
Sudden eye pain, marked redness, or a rapid drop in vision also needs prompt review. These symptoms can reflect several serious problems, from pressure spikes to inflammation or infection. You do not need to work out which one it is before you act.
Blurred vision that develops over months can fit a cataract. Vision that falls over minutes or hours is a different category. If you cannot see clearly enough to function, or if one eye changes dramatically, treat it as urgent.
After being told you may have cataracts, glaucoma, or a retinal disease
If you have already been told you may have cataracts, glaucoma, macular degeneration, diabetic retinopathy, or another retinal condition, specialist assessment should not drift to the bottom of the list. Cataracts are not always emergencies, but once they are affecting reading, driving, or independence, you need a proper surgical opinion. Glaucoma and retinal disease deserve even less delay.
The goal is not panic. The goal is speed with judgment. When the local assessment suggests a structural eye problem, the next specialist step should be booked with intent.
New flashes and floaters should be treated as a same-day eye problem, not a routine checkup.
What are the common questions about ophthalmologists?
Most practical questions are about access: do you need a referral, can family members of different ages be seen, and what happens if you live far from a specialist centre?
Do I need a referral?
A referral depends on your local health system and, in some cases, your insurer. Many patients are referred by an optometrist or a general practitioner because that route packages the problem clearly: symptoms, timing, test results, and urgency. That can speed triage.
If you already have scans, letters, or a record of prior eye surgery, bring them. A referral is not just paperwork. It is context. And in eye disease, context saves time.
Can ophthalmologists treat children and adults?
Yes. Ophthalmology covers both adults and children, although some ophthalmologists focus on particular age groups or subspecialties. Practices commonly list blocked tear duct care in children among their services, while adults more often present with cataracts, glaucoma, diabetic retinopathy, or macular degeneration.
If a child has a red eye, tearing, or an eyelid or visual concern, specialist assessment may still be appropriate. The same is true for older adults whose symptoms are brushed off as “just age.” Age changes vision, but age does not explain every symptom.
What if I live in a rural or regional area?
If you live in a rural or regional community, you may need to travel for retinal surgery, advanced cataract treatment, or complex ophthalmic imaging. That is common. It is also worth planning properly. Ask what can be done locally, what must be done by a specialist, and whether follow-up can be shared closer to home after the critical treatment is completed.
For patients in the Hills district, Canberra, Liverpool, Randwick, and surrounding regional areas, seeing an ophthalmologist such as Dr Rahul Dubey can shorten the path from diagnosis to treatment for cataracts and retinal disease. Bring your referral, medication list, and any scans. Make the first visit count.
If local care can’t address a complex retinal or cataract issue, the right specialist visit is worth the trip.
The right eye doctor at the right moment can protect sight, not just sharpen a prescription.
If you came here asking what is a ophthalmologist, you now have the practical answer: optometrists handle routine vision care, while ophthalmologists diagnose disease, prescribe treatment, and perform surgery for cataracts, glaucoma, and retinal problems.
When your vision changes suddenly, or a local exam suggests something more serious, what next step would give you the fastest path to preserving sight?




Comments