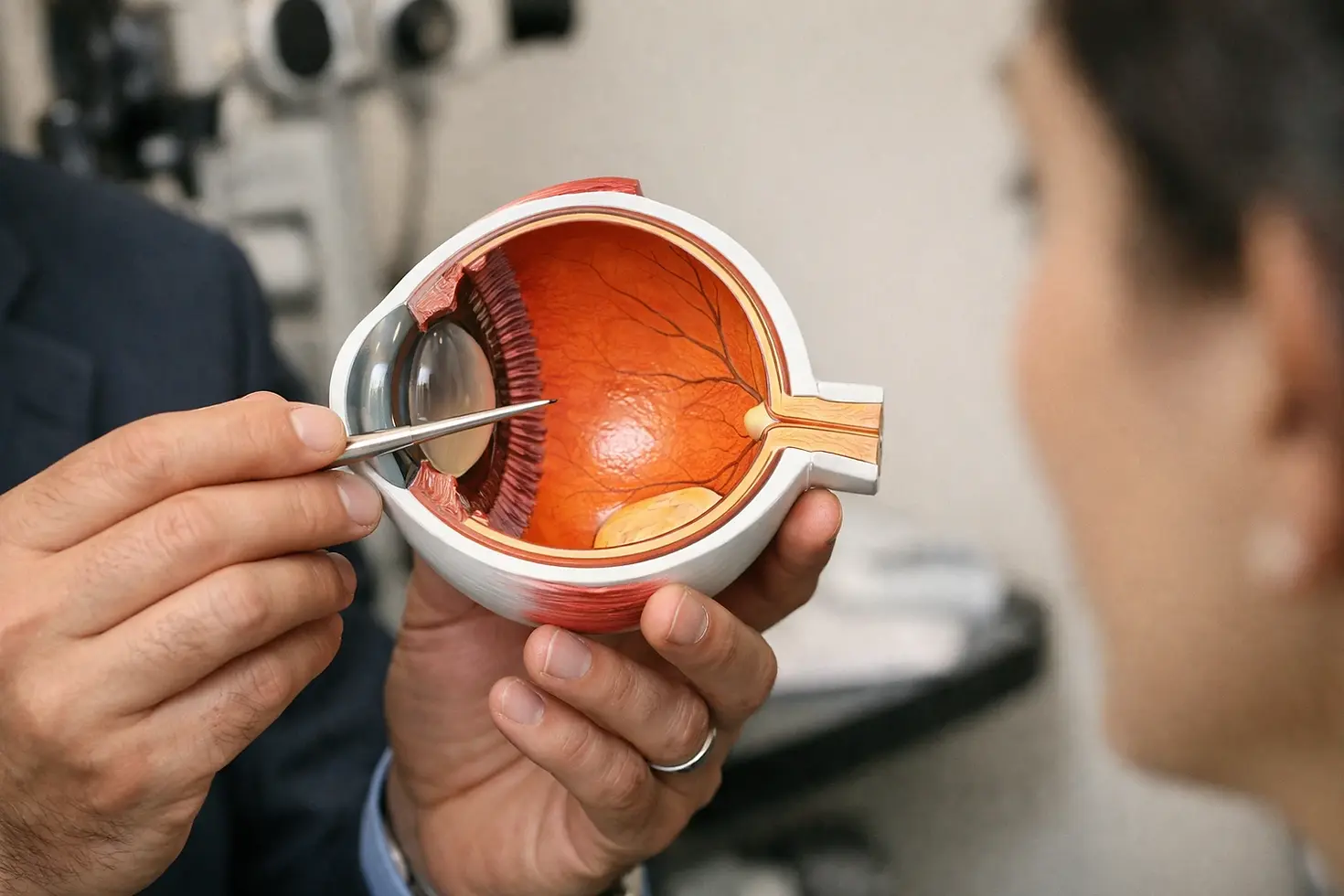
What is pars plana and pars plicata
- Mar 7
- 8 min read
If you have been told about the pars plana or the pars plicata during an eye consultation, you may wonder what these terms really mean and why they matter. The pars plana is the flat, posterior part of the ciliary body, while the pars plicata is the folded, anterior part with ciliary processes. Understanding where each sits and what each does can help you make informed decisions about retinal and cataract care. Moreover, a well-structured checklist can turn complex anatomy into practical steps you can follow with confidence.
This guide is tailored for people in the Hills district, Canberra, Liverpool, Randwick, and surrounding rural and regional communities who need clear, trustworthy information. You will find concise actions, supportive examples, and local context so you can prepare for appointments, discussions, and potential procedures. Because the stakes are your sight, clarity matters from the first question you ask to the last box you tick.
Pre-work checklist: Understand the pars plana and pars plicata
Before you commit to any plan, ground yourself in the essentials. These structures live within the ciliary body, part of the uvea, and are central to safe, effective care of the back of the eye. When you grasp how the pars plana and pars plicata differ, you will better understand why surgeons select certain approaches, and why imaging and timing influence outcomes. Use the actions below to build a firm foundation you can bring into your consultation with Dr Rahul Dubey.
Identify each structure clearly. Learn that the pars plicata is the front, folded portion of the ciliary body with ciliary processes that produce aqueous fluid, while the pars plana is the flatter, back portion closer to the retina and vitreous cavity.
Place them spatially in your mind. Visualize the iris and the sclera meeting at the limbus, then imagine the pars plicata just behind the iris and the pars plana just behind the pars plicata.
Connect anatomy to decisions. Recognize that the pars plana is commonly used as the safest doorway to the posterior segment for surgery on the vitreous and retina because it avoids damage to the lens and ciliary processes.
List your symptoms precisely. Note new floaters, flashes, a curtain of vision loss, distorted central vision, or blurred night driving, and document when they began and how they are changing.
Gather your medical details. Bring a list of medications, especially for diabetes and blood pressure, recent blood sugar results if applicable, and any history of eye surgery or trauma.
Request appropriate imaging. Ask about optical coherence tomography for macula evaluation, widefield retinal photography for the periphery, and ultrasound if the view is cloudy due to cataract or hemorrhage.
Clarify travel logistics if you live regionally. Plan how you will reach clinics in the Hills district, Canberra, Liverpool, or Randwick, and discuss urgent pathways for conditions like a retinal detachment where time matters.
Understand cataract implications. If a cataract blocks the view to the retina, discuss whether advanced cataract surgery including femtosecond laser should be combined or sequenced with retinal surgery for the most efficient and safest care.
Use this quick comparison to lock in the key differences and where each structure influences treatment choices.
If you feel overwhelmed, remember that you do not have to master every detail. The goal is to arrive at your appointment with the right questions so you and your specialist can decide on a pathway together. In Dr Rahul Dubey’s clinics across the Hills district, Canberra, Liverpool, and Randwick, the team translates this anatomy into a clear plan, and supports rural and regional patients with streamlined pathways.
Execution checklist: Plan and act on care around the pars plana
Once the groundwork is set, it is time to execute a plan aligned with your diagnosis, life, and preferences. Good execution is not just surgical finesse; it is timing, coordination, and communication. The following actions reflect current best practices and the on-the-ground realities for people balancing travel, family, and work.
Confirm the diagnosis with precise imaging. Use optical coherence tomography to diagnose macular hole, epiretinal membrane, or macular edema, and consider widefield imaging for diabetic retinopathy or peripheral tears.
Stratify urgency. Treat a retinal detachment as urgent, often requiring same-day or next-day action. Address vitreous hemorrhage, macular hole, and epiretinal membrane on a prioritized timetable informed by your visual needs.
Discuss the entry site. Ensure your surgeon explains how the pars plana provides access to the posterior segment while preserving the lens and ciliary structures, and how the entry is positioned relative to the limbus.
Plan anesthesia thoughtfully. Choose local anesthesia with sedation or general anesthesia based on your comfort, medical history, and the complexity of the procedure.
Coordinate with cataract care when needed. If a cataract obscures the view or is likely to progress, consider advanced cataract surgery including femtosecond laser. Combining or staging procedures can reduce total recovery time and optimize accuracy.
Minimize incision size. Favor small, self-sealing incisions to reduce discomfort and speed recovery, supporting quicker return to daily activities.
Confirm infection control steps. Review preoperative antisepsis and postoperative antibiotics, and follow protocols meticulously to safeguard against rare but serious infections.
Align the plan with your location. If you live regionally, organize transport and accommodation ahead of time, and use telehealth follow-up where appropriate to reduce travel burden.
To make sense of technical placement details, this table shows typical guidance for instrument entry relative to the limbus, which helps protect the lens and ciliary body. Your surgeon will individualize these numbers to your eye size and lens status.
In practice, multiple published series suggest high anatomic success for modern small-incision surgery on the vitreous and retina, frequently above nine out of ten cases for common indications when performed by experienced teams. Outcomes are even better when cataract and retina plans are coordinated early, and when follow-up is reliable. Under Dr Rahul Dubey’s care, retinal surgery is performed expertly and urgently, and cataract surgery is no gap, with pathways designed for patients from metropolitan centers and regional communities alike.
Validation checklist: Confirm progress and protect results
Good surgery and medical treatment are only the first steps. Validation ensures that healing goes to plan, vision stabilizes, and preventable risks are managed early. By testing vision, inspecting the retina, monitoring intraocular pressure, and reviewing imaging, you and your clinician create a feedback loop that keeps you on track. Use the checks below to stay proactive.
Track your functional vision. Check reading, face recognition, and driving confidence at regular intervals, and note any sudden changes such as a dark shadow or an increase in floaters.
Attend scheduled reviews. Keep appointments in the Hills district, Canberra, Liverpool, or Randwick, and use telehealth where appropriate for rural and regional access between in-person visits.
Measure intraocular pressure. Ensure your clinician assesses eye pressure at each visit to detect pressure spikes or drops that may require medication adjustment.
Repeat imaging when indicated. Use optical coherence tomography to verify macular hole closure or epiretinal membrane removal, and use widefield imaging to confirm stable peripheral retina after repair.
Check wound integrity. Ask for confirmation that entry points through the pars plana are sealed and that there is no leakage, redness, or tenderness that suggests inflammation.
Audit medications and dosing. Verify that anti-inflammatory drops, pressure-lowering drops, and other medications are taken as prescribed, and reconcile changes with your general practitioner if needed.
Review systemic risk factors. Keep diabetes and blood pressure controlled because good systemic health supports ocular healing and reduces recurrence risk.
Escalate promptly if red flags arise. Seek urgent care for increasing pain, sudden blur, a curtain of vision loss, nausea with eye pain, or rapidly rising floaters and flashes.
Validation is not about perfection; it is about catching small deviations early. Studies in retinal care consistently show that adherence to review schedules and medication plans improves outcomes and reduces complication rates. With coordinated pathways across Dr Rahul Dubey’s locations and thoughtful support for regional patients, this validation step becomes practical and sustainable.
Common misses: Avoid pitfalls that delay recovery or reduce results
Even well-informed patients can stumble over a few recurring challenges. These misses are avoidable with a little foresight, a few direct questions, and a willingness to act early. Consider how many of these apply to you, and address them before they cost you time or vision.
Confusing location and function. Do not mix up the pars plicata and the pars plana. The folded, fluid-producing pars plicata is not used for posterior entry, while the flatter pars plana is the standard entry zone for instruments.
Waiting too long with symptoms. A fresh retinal detachment, sudden showers of floaters, or a curtain-like shadow requires urgent assessment. Hours and days matter.
Skipping cataract planning. If a cloudy lens blocks the view to the retina, do not postpone cataract planning. Combining advanced cataract surgery including femtosecond laser with retinal steps may speed recovery and enhance precision.
Underestimating travel friction. Rural and regional patients often need a plan for transport and accommodation. Do not let logistics be the reason you miss a crucial window for care.
Overlooking systemic health. Poorly controlled diabetes or blood pressure can derail healing. Bring your latest results and align care with your broader health team.
Misplacing follow-up intervals. Visual improvement can be gradual. Keep each follow-up until your clinician confirms that your retina is stable and your eye pressure is on target.
Focusing on tools instead of outcomes. While modern technology is valuable, the aim is durable vision and a stable retina. Prioritize plans that align with your daily life and long-term goals.
Failing to ask about the plan for both eyes. If one eye needs urgent care, discuss surveillance and prevention for the fellow eye, especially with conditions like lattice degeneration or diabetic retinopathy.
These pitfalls are common because the journey can feel opaque. Clear language, precise imaging, and a stepwise plan will cut through the confusion. In Dr Rahul Dubey’s practice, you will find the full spectrum of care under one roof, including medical and surgical management of vitreomacular disorders, surgery for floaters, micro surgery for macular hole and epiretinal membrane, management of retinal detachment and diabetic retinopathy, and expertise in inflammatory eye disease and age-related macular degeneration, all with a strong commitment to rural and regional services.
Conclusion
The core promise of this guide is simple: when you understand the pars plicata and the pars plana, your decisions become clearer, faster, and safer.
Imagine navigating care with confidence, from accurate imaging to expertly timed surgery, with seamless coordination across the Hills district, Canberra, Liverpool, Randwick, and regional pathways designed around your life.
In the next 12 months, what would it mean for your work, family, and independence if you could protect or restore vision by acting early and choosing the right plan for the pars plana?
Appendix: Practical examples grounded in local care
Real-world scenarios can translate anatomy into decisions you can make today. The following brief examples show how Dr Rahul Dubey’s comprehensive services support people across different needs and postcodes, from rapid triage to meticulous planning.
Macular hole in a retiree from the Hills district. After optical coherence tomography confirms a full-thickness macular hole, coordinated scheduling allows surgery through the pars plana with membrane peeling. Visual potential and activity goals shape the timeline, and follow-up ensures hole closure and controlled intraocular pressure.
Diabetic vitreous hemorrhage in a farmer from a regional town. Ultrasound confirms an attached retina. Timely surgery via the pars plana clears blood, while diabetic management is tightened with the general practitioner. Telehealth reduces travel for interim reviews between visits to Canberra or Liverpool.
Advanced cataract with epiretinal membrane in a teacher from Randwick. Planning includes advanced cataract surgery including femtosecond laser and a coordinated retinal procedure. The approach improves visual clarity, reduces time in care, and limits total recovery, with imaging used to validate progress after each step.
Across these examples, the message holds: place anatomy in context, act on a checklist, and leverage a team that delivers urgent retinal surgery when every hour counts. When you combine that with precision cataract pathways, you are well positioned for durable, high-quality vision.




Comments