How Long Does a Retinal Tear Take to Heal: A Step‑By‑Step Guide
- Jan 11
- 17 min read
Imagine you wake up one morning, notice a sudden dark spot in the corner of your vision, and the eye doctor tells you it’s a retinal tear. That moment can feel like a punch to the gut, especially when you’re juggling work, family, and that weekend surf session you’ve been looking forward to.
You’re probably wondering, how long does a retinal tear take to heal? The short answer is: it varies, but most people see significant healing within a few weeks if they follow the right post‑procedure care.
In our experience at the Sydney retina clinic, the healing timeline hinges on three factors: the size of the tear, the treatment method used, and how diligently you stick to post‑op instructions.
If the tear is small and we seal it with laser retinopexy, you’ll usually notice improvement in 7‑10 days, and the retina continues to re‑attach over the next 2‑3 weeks. Larger tears that need a scleral buckle or vitrectomy can take 4‑6 weeks for the retina to stabilise, and full visual recovery may stretch to two months.
But healing isn’t just about the clock. Your eyes need protection from strain, bright lights, and heavy lifting. Simple steps like wearing UV‑blocking sunglasses, avoiding vigorous sports for the first week, and using prescribed eye drops can shave days off the recovery.
So, what can you do right now? Keep the appointment for your follow‑up, track any new floaters or flashes, and don’t hesitate to call us if you notice worsening vision. Early detection of complications saves time and vision.
Remember, every retina is unique, and we’ll tailor the plan to your lifestyle—whether you’re a busy professional in the CBD or a parent shuttling kids to school in the suburbs.
Stick with the plan, and you’ll be back to reading the morning paper or spotting dolphins off Bondi in no time.
TL;DR
Healing a retinal tear depends on size, treatment type, and post‑op care; small laser‑sealed tears improve in 7‑10 days, larger repairs take up to two months.
Wear UV‑blocking sunglasses, skip heavy lifting, keep follow‑up appointments, and you’ll be back reading the paper or spotting dolphins off Bondi in weeks soon.
Step 1: Identify Your Retinal Tear Type
First thing’s first – you need to know what you’re dealing with. A retinal tear isn’t a one‑size‑fits‑all problem; the size, shape and location all dictate how fast it will heal and what treatment you’ll need.
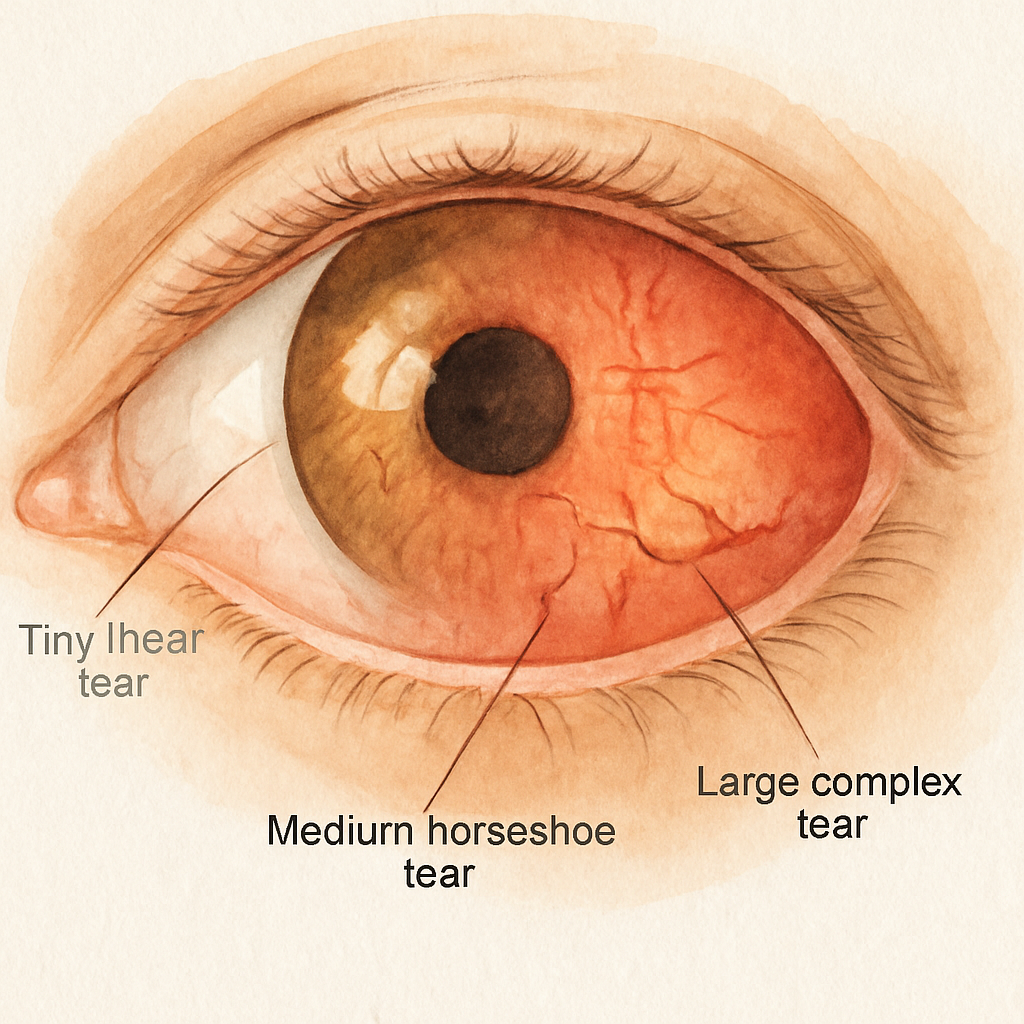
When you walk into our clinic in Sydney, the first thing I do is a dilated eye exam. With a wide‑field retinal camera I can see whether the tear is a tiny nick at the peripheral edge or a larger horseshoe‑shaped break closer to the macula. That visual map is the roadmap for the rest of your recovery.
Here’s a quick cheat‑sheet you can use at home (but don’t skip the professional exam!):
Micro‑tear (≤1 disc diameter)– usually a clean, linear break. Often sealed with laser retinopexy.
Medium tear (1‑3 disc diameters)– may need a combination of laser and a short‑term gas bubble (pneumatic retinopexy).
Large tear (>3 disc diameters) or multiple breaks– typically requires a scleral buckle or vitrectomy.
Why does this matter? Because the larger the tear, the more tissue needs to re‑attach, and the longer the healing timeline stretches. A micro‑tear can start sealing in a matter of days, while a vitrectomy for a big tear might keep you on a light‑restriction regimen for six weeks or more.
Let’s walk through a real‑world scenario. Sarah, a 42‑year‑old surfer from Bondi, woke up with a sudden curtain‑like shadow. In the exam we spotted a 0.8‑disc‑diameter tear near the superior retina. Because it was small, we opted for laser retinopexy. She noticed visual improvement in about eight days and was back on the beach in three weeks.
Contrast that with Mark, a 58‑year‑old accountant who had a 4‑disc‑diameter horseshoe tear involving the macula. We performed a vitrectomy with a silicone oil tamponade. His vision stabilized around week five, but he needed to avoid heavy lifting and bright screens for eight weeks before feeling normal again.
These stories illustrate the core emotional experience: uncertainty about how long you’ll be “out of the game.” Knowing the tear type lets you set realistic expectations and plan your life accordingly.
How do you identify the type yourself? You can’t, but you can recognise warning signs that point to a bigger problem:
Sudden increase in floaters – especially if they look like black specks marching across your vision.
Flashes of light – often described as “camera flash” in the periphery.
Partial loss of peripheral vision – a shadow or curtain that doesn’t move with your eyes.
If any of these appear, book an urgent appointment. Early detection means a smaller tear, a simpler procedure, and a faster return to normal.
Once the tear is classified, we move to the next step: choosing the right treatment. For a deeper dive on what causes these tears in the first place, check out our guide on Understanding retinal tear causes: A clear guide . It explains risk factors like high myopia, trauma, and age‑related vitreous changes – knowledge that can help you prevent future tears.
Actionable checklist for today:
Schedule a dilated retinal exam within 24‑48 hours of symptom onset.
Write down any new floaters, flashes, or shadow changes.
Avoid rubbing your eyes and limit exposure to bright sunlight until you’re seen.
Prepare a list of current medications – some eye drops can affect post‑procedure healing.
Remember, the sooner we pin down the tear type, the sooner we can map out a clear healing timeline. And that timeline is the first step toward getting back to reading the morning paper or catching that wave at Bondi.
Step 2: Understand the Healing Process
Now that you know what kind of tear you’re dealing with, the next question is: how long does a retinal tear take to heal? The answer isn’t a one‑size‑fits‑all number – it depends on the treatment you receive, how your eye reacts, and how closely you follow post‑op care.
Let’s break it down so you can picture the timeline in real life.
What the body does after the procedure
When we seal a tear with laser retinopexy, a tiny scar forms around the break. That scar acts like a fence, keeping the retina glued to the back of the eye. In most cases you’ll start noticing less floaters and fewer flashes within the first week.
If a gas bubble is used – as in pneumatic retinopexy or vitrectomy – your eye needs to stay face‑down for a while. The bubble presses against the retina, holding it in place while the tissue heals. The American Academy of Ophthalmology explains that the face‑down period can last from a few days to several weeks, depending on the bubble size and the surgeon’s plan.
Typical recovery windows
Laser retinopexy: most patients see a noticeable improvement in vision by day 7‑10. Full re‑attachment continues over the next 2‑3 weeks. If you’re curious about what to expect after laser, check out our guide on Laser Retinopexy Recovery Time: What to Expect After the Procedure for day‑by‑day milestones.
Pneumatic retinopexy: the gas bubble typically remains for 1‑2 weeks. During that time you’ll need to keep your head tilted or face‑down, especially while sleeping. Most people can resume light activities after about 10 days, but you should avoid heavy lifting and bright screens until the bubble fully dissolves.
Scleral buckle: the buckle is a permanent silicone band placed around the eye. Healing of the retinal tissue takes about 4‑6 weeks, and you’ll need to wear a protective shield for the first few days. Vision stabilises around week 5, but fine‑tuning of glasses may take a little longer.
Vitrectomy: this is the most involved surgery. The eye is filled with a tamponade (gas or silicone oil) and the internal gel is removed. Recovery can stretch to 6‑8 weeks, with the oil staying in place for months if used. Patients often report gradual clarity improvement rather than a sudden “aha!” moment.
Actionable steps to speed healing
Follow positioning instructions exactly. Use a face‑down pillow or chair if your surgeon recommends it – even short lapses can delay the bubble’s work.
Protect your eyes from bright light. UV‑blocking sunglasses aren’t just a fashion statement; they reduce phototoxic stress on the healing retina.
Stick to prescribed eye drops. Anti‑inflammatories and antibiotics keep swelling down and prevent infection.
Avoid heavy lifting, straining, or vigorous exercise for the first 1‑2 weeks. Think of your eye as a fresh‑cut garden – you wouldn’t run a lawn mower over it.
Keep a symptom diary. Note any new flashes, increased floaters, or pain and call us immediately – early detection of a re‑detachment can save weeks of recovery.
Here’s a quick checklist you can print out and tape to your fridge:
Wear UV sunglasses whenever you’re outside.
Use the face‑down pillow every night for the first 5 days.
Apply eye drops at the same times each day.
Log any visual changes in a notebook.
Schedule your follow‑up appointment before the week is over.
Real‑world snapshots
Sarah, a 38‑year‑old graphic designer, had a tiny peripheral tear sealed with laser. She followed the drop regimen, wore sunglasses, and was back to designing on her laptop by day 12. She says the biggest surprise was how quickly her eye felt “normal” again – she almost forgot she’d had surgery.
Mark, a 60‑year‑old accountant, required a vitrectomy with silicone oil. He kept a face‑down pillow for two weeks, avoided his morning jog, and used the prescribed steroid drops. By week 6 his vision steadied, and he could finally read the financial headlines without squinting. He notes that the extra patience paid off – his retina stayed attached and he avoided a second operation.
Both stories highlight the same theme: the healing timeline shortens when you treat the post‑op plan like a contract with your eye.
Beyond the clinic – protecting your vision long term
Even after the retina has re‑attached, you’ll still need to think about protective eyewear. Prescription sunglasses can reduce glare and UV exposure, which are proven to slow age‑related retinal wear. If you’re shopping for the right pair, Does Insurance Cover Prescription Sunglasses? A Complete Guide breaks down what to look for and how to claim.
And if you’re a small‑business owner or a solo practitioner looking to improve your online booking system, a solid website platform can make it easier for patients to schedule follow‑ups. Shopify Alternatives for Australian Small Businesses offers a quick rundown of options that work well for health‑care providers.
Bottom line: healing a retinal tear is a step‑by‑step journey. By understanding the biology, respecting positioning, and staying on top of meds, you can shave days off the timeline and get back to the things you love – whether that’s surfing at Bondi or reviewing spreadsheets in the CBD.
Step 3: Choose the Right Treatment
Alright, you’ve pinned down the tear type – now the real decision begins. Which treatment will give you the fastest, safest road back to clear vision? It feels a bit like picking a surfboard: the right shape, size, and flex make all the difference, and the wrong choice can leave you wiping out.
Match the tear to the method
Here’s the quick cheat‑sheet we use in our Sydney clinic:
Laser retinopexy– best for micro‑tears (≤1 disc diameter). It’s an office‑based laser zap that creates a tiny scar fence around the break.
Pneumatic retinopexy– works for medium tears (1‑3 disc diameters). A gas bubble is injected and you stay face‑down for a few days.
Scleral buckle– reserved for larger or multiple tears. A silicone band is sutured around the eye to give the retina a supportive hug.
Vitrectomy– the heavyweight option for complex, macula‑involving tears. The gel inside the eye is removed and replaced with gas or silicone oil.
Choosing the right tool isn’t just about size; it’s also about your lifestyle. A surfer who can’t be face‑down for a week might lean toward laser, while an accountant with a large horseshoe tear may need the stability of a vitrectomy.
What the numbers say
Data from recent studies (2024‑2025) show average visual improvement timelines:
Laser retinopexy: noticeable change by day 7‑10, full re‑attachment by week 3.
Pneumatic retinopexy: bubble clears in 10‑14 days, functional vision usually returns by week 4.
Scleral buckle: retina stabilises around week 5, fine‑tuning of glasses may extend to week 6‑8.
Vitrectomy: gradual clarity over 6‑8 weeks, with silicone oil sometimes staying months.
These figures line up with what we see in our practice – the bigger the intervention, the longer the patience required.
Actionable steps to pick your treatment
Ask the right questions at your appointment.“Will I need to stay face‑down?” “How soon can I return to work?” “What’s the risk of re‑detachment?”
Consider your daily routine.If you’re a small‑business owner juggling client calls, a short‑term gas bubble might clash with your schedule.
Review recovery aids.UV‑blocking sunglasses, prescribed eye drops, and a comfortable face‑down pillow can make the hardest days easier.
Plan for follow‑ups.Our clinic typically schedules the first check‑up within a week, then another at the 4‑week mark to confirm re‑attachment.
Get a clear timeline.For a deeper dive on vitrectomy timelines, see our guide How Long Does a Vitrectomy Take? A Step‑by‑Step Guide .
And don’t forget to write down any new floaters or flashes in the days after the procedure – they’re the early warning lights that tell us whether the retina is still holding together.
Real‑world snapshots
Take Maya, a 35‑year‑old graphic designer who lives in the CBD. She had a 0.9‑disc‑diameter tear near the superior periphery. We sealed it with laser retinopexy. By day 9 she reported “the curtain’s lifting,” and by week 2 she was back to Illustrator without glare. Her quick return was helped by strict UV‑sunglass use and a simple drop schedule.
Contrast that with Tom, a 60‑year‑old accountant from Parramatta. He presented with a 4‑disc‑diameter horseshoe tear involving the macula. A vitrectomy with silicone oil was necessary. He spent two weeks on a face‑down pillow, avoided his usual morning jog, and kept a daily symptom log. At the 6‑week visit his vision had stabilised, and the oil was removed at week 12. He says the extra weeks felt “like a marathon,” but the final outcome was worth it – his vision stayed stable and he avoided a second surgery.
Expert tip: tailor the treatment to your risk factors
High myopia, previous eye surgery, or a history of retinal detachment all push us toward the more aggressive options because the retina is a bit more fragile. In those cases, we often recommend a scleral buckle or vitrectomy even for medium‑sized tears, just to give that extra safety net.
And here’s a quick checklist you can print:
Ask: face‑down required? (yes/no)
Confirm: how many drops per day?
Note: any activity restrictions?
Schedule: first follow‑up within 7 days.
Prepare: UV sunglasses and a comfortable pillow.
Running a clinic? A side note on IT support
If you’re managing a retina practice, the tech side matters too. Secure IT infrastructure keeps patient data safe and ensures your online booking runs smoothly. A practical read on that is Understanding IT Outsourcing Services: A Practical Guide for SMBs .
Bottom line: the right treatment isn’t a one‑size‑fits‑all answer. It’s a balance between tear characteristics, your personal schedule, and the support you have at home. By asking the right questions, planning your recovery steps, and leaning on our expertise, you’ll shave weeks off the timeline and get back to the things that matter – whether that’s a surf session at Bondi or a meeting with a client in the CBD.
Step 4: Compare Healing Times by Treatment
Alright, you’ve picked a treatment – now let’s see how long each one actually takes to heal. The difference between a week and six weeks can feel huge when you’re planning a surf session or a client meeting.
First up, laser retinopexy. In our Sydney clinic we see micro‑tears seal in about 7‑10 days, with the retina continuing to stabilise over the next two weeks. Most patients report a noticeable drop in floaters by day 5 and can return to light screen work by the end of week 2.
Next, pneumatic retinopexy. The gas bubble does the heavy lifting, but you’ll need to stay face‑down for a few days. The bubble usually disappears in 10‑14 days, and you can ease back into normal activities by week 3. If you skip the positioning, the bubble can shift and delay healing.
Now, the scleral buckle. This is where the Scleral Buckle Recovery Time: What to Expect and How to Heal Faster guide gets useful. Healing takes roughly 4‑6 weeks. You’ll wear a protective shield for the first few days, and vision typically stabilises around week 5. Heavy lifting should stay off the table for at least two weeks.
Finally, vitrectomy – the heavyweight option for large, macula‑involving tears. Recovery can stretch to 6‑8 weeks, sometimes longer if silicone oil is left in place. Patients often notice gradual clarity improvement rather than a sudden “aha” moment. Keep a symptom diary; any new flashes after week 4 should trigger a call.
So, how do you choose? Think about your daily routine, how long you can stay face‑down, and how quickly you need visual stability. If you’re a busy accountant in the CBD, a laser might get you back to the spreadsheet faster. If you’re a surfer who can’t tolerate face‑down time, a buckle might be the sweet spot despite the longer timeline.
Below is a quick comparison table you can print out. It lines up the treatment, typical healing window, and a top tip you can start using today.
Treatment | Typical Healing Window | Key Patient Tip |
Laser Retinopexy | 7‑10 days for noticeable improvement; 2‑3 weeks for full re‑attachment | Wear UV‑blocking sunglasses daily; keep eye drops on schedule |
Pneumatic Retinopexy | 10‑14 days for bubble resolution; 3‑4 weeks for functional vision | Use a face‑down pillow every night; avoid bending over |
Scleral Buckle | 4‑6 weeks for retinal stabilisation; vision steadies around week 5 | Shield eye for first 48 hrs; limit lifting >5 kg |
Vitrectomy | 6‑8 weeks (oil may stay months) | Log any new flashes; report pain immediately |
Remember, the numbers are averages. Your own healing curve can be faster if you stick to the post‑op plan religiously. Keep that symptom diary, protect your eyes from bright light, and don’t skip follow‑up appointments – they’re the checkpoints that let us catch any setbacks early.
Bottom line: compare the timelines, match them to your lifestyle, and use the tips above to shave days off the journey. You’ll be back to reading the paper on the Bondi promenade or reviewing contracts in the CBD before you know it.
Step 5: Support Your Recovery at Home
Now that you’ve chosen a treatment and know the typical healing windows, the real work begins inside your own four walls. Your eye is a delicate garden – it needs the right amount of sun, water and protection to bloom back to health.
So, what does “supporting recovery at home” actually look like? It’s a mix of practical habits, a few pieces of gear, and a mindset that treats every day like a mini‑appointment with your retina.
Create a safe visual environment
First, think about lighting. Bright fluorescents or harsh sunlight can irritate a freshly sealed retina. Keep windows covered with UV‑blocking curtains in the morning and wear sunglasses even when you’re just stepping out for the mail.
And don’t forget your indoor glow. Swap harsh desk lamps for a soft, warm LED bulb. If you work on a computer, use the built‑in “night shift” mode or a blue‑light filter – it reduces strain without sacrificing readability.
Gear up for comfort
Most surgeons will give you a face‑down pillow or a specialised positioning wedge. It sounds odd, but think of it like a yoga block – it holds your eye in the right spot while the gas bubble does its job.
Here’s a quick checklist of what to have on hand:
UV‑blocking sunglasses (polarised are a bonus)
Prescribed eye‑drop schedule written on a sticky note
Face‑down pillow or a firm travel‑neck pillow
Water bottle within arm’s reach – staying hydrated helps tissue repair
Notebook or a simple app to log any new flashes, floaters or pain
In our clinic we often hand patients a one‑page “Recovery at Home” sheet that mirrors this list. If you missed that, you can download a similar guide from our eye‑surgery recovery guide – it breaks down each step in plain language.
But gear alone isn’t enough. Your daily routine needs a few small tweaks to keep the healing process on track.
Daily habits that speed healing
1.Stick to the drop timetable.Missing a dose is like skipping a beat in a song – the rhythm gets off and your retina may take longer to seal.
2.Limit head‑down activities.Bending over to tie your shoes, lifting a heavy ute, or intense yoga inversions can raise intra‑ocular pressure. Keep these to a minimum for the first two weeks.
3.Stay hydrated and nourished.Foods rich in omega‑3 fatty acids – think salmon, walnuts and chia seeds – support retinal health. A simple glass of water every hour also keeps the ocular surface lubricated.
4.Protect against accidental bumps.Pad sharp corners on coffee tables, move rugs that could cause a slip, and consider a soft eye shield for the first 48 hours if your surgeon recommended one.
5.Get enough rest.Sleep is when most cellular repair happens. Aim for 7‑9 hours of uninterrupted rest, and try to keep your head slightly elevated to reduce swelling.
Does any of this feel overwhelming? It can, especially when you’re juggling work calls, school runs and a weekend surf session. The trick is to batch‑process: set a reminder for eye‑drops, place your sunglasses on the front door hook, and keep your notebook on the nightstand. Small cues turn a chore into an automatic habit.
When to call the clinic
Even the best home plan can’t replace professional oversight. If you notice any of these red flags, pick up the phone right away:
Sudden increase in floaters or a new “cobweb” feeling
Sharp pain behind the eye, especially if it worsens at night
Rapid loss of vision or a new curtain‑like shadow
Persistent redness or discharge
Early intervention can shave days or even weeks off your overall timeline, because we can address a re‑detachment before it becomes a major setback.
Finally, give yourself credit for the progress you make each day. Healing a retinal tear isn’t a sprint; it’s a steady climb. Celebrate the small wins – like the first time you can read the news without squinting, or the moment you can walk the dog without worrying about a sudden jolt.

Stick to these home‑based strategies, and you’ll find that “how long does a retinal tear take to heal” becomes less of a mystery and more of a manageable countdown.
FAQ
How long does a retinal tear take to heal after laser retinopexy?
In most cases you’ll notice a visible improvement within 7‑10 days. The tiny scar that the laser creates continues to tighten the retina over the next two to three weeks, so full stability usually arrives around day 21. We see many Sydney patients back to reading the news by the second week, as long as they stick to drops and UV protection.
What is the typical recovery time for pneumatic retinopexy?
The gas bubble stays in place for about 10‑14 days. During that window you’ll need to stay face‑down for several hours a day, which can feel odd but speeds up the seal. Functional vision often returns by week 3‑4, and most people feel comfortable resuming light activities after the bubble dissolves. Keep your eye drops on schedule and avoid heavy lifting.
How many weeks does a scleral buckle procedure usually require for healing?
Healing after a scleral buckle tends to follow a 4‑6‑week curve. The retina generally stabilises around week 5, and you’ll notice clearer vision shortly after. Protect the eye with the shield we give you for the first 48 hours, limit lifting over 5 kg, and keep up with anti‑inflammatory drops. Most patients can return to normal work by the end of week 6.
What should I expect if I undergo a vitrectomy for a large retinal tear?
Vitrectomy is the most involved option, so recovery can stretch to 6‑8 weeks, sometimes longer if silicone oil is left in place. Vision improves gradually rather than in a single “aha” moment. Log any new flashes or pain, keep your head slightly elevated, and use the prescribed steroid regimen. By week 8 many patients report stable vision and can resume most daily tasks.
When is healing taking longer than expected?
If you notice a sudden surge of floaters, a new curtain‑like shadow, increasing pain, or persistent redness after the first week, it could signal a re‑detachment or inflammation. Call the clinic immediately – early intervention can shave days or weeks off the overall timeline. Also, missing eye‑drop doses or breaking face‑down positioning can delay the seal.
Can I do anything to speed up the healing process?
Yes. Stick to the drop schedule without gaps, wear UV‑blocking sunglasses whenever you’re outdoors, stay hydrated, and avoid activities that raise intra‑ocular pressure (heavy lifting, vigorous yoga inversions). A simple symptom diary helps you spot changes early. In our experience, patients who treat the post‑op plan like a daily checklist often recover a week sooner.
Conclusion
If you’ve made it this far, you already know that “how long does a retinal tear take to heal” isn’t a one‑size‑fits‑all answer. The timeline bends around the tear size, the treatment you choose, and how faithfully you follow post‑op instructions.
In short: laser retinopexy can give you noticeable improvement in a week and full stability by three weeks; pneumatic retinopexy usually wraps up in three to four weeks; a scleral buckle settles around five weeks; and vitrectomy can stretch to six‑to‑eight weeks, sometimes longer with silicone oil.
What matters most is what you do every day. Keep your eye‑drop schedule tight, wear UV‑blocking sunglasses, log any new flashes, and respect face‑down positioning when it’s required. Those tiny habits shave days off the curve and keep complications at bay.
So, what’s the next step? Grab the checklist we’ve shared, set a reminder for your drops, and book that follow‑up appointment before the week is out. Your retina will thank you, and you’ll be back to reading the paper on the Bondi promenade sooner than you think.
Remember, healing is a partnership – you, your surgeon, and the simple routine you stick to. Stay patient, stay vigilant, and let the eye do its quiet work.






Comments