Do Eye Injections Hurt? What You Need to Know Before Your Treatment
- Jan 16
- 16 min read
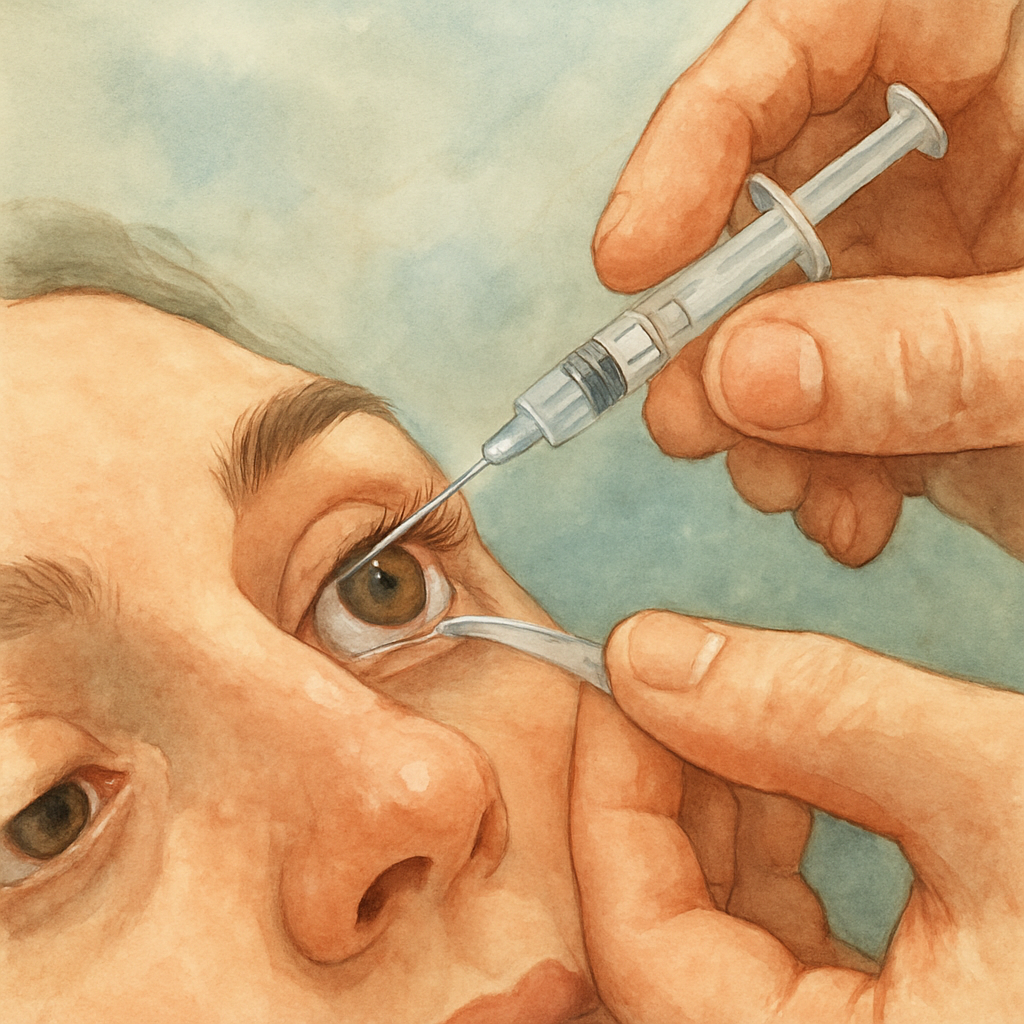
Imagine sitting in the waiting room of our Sydney clinic, the hum of the air‑conditioner mixing with the faint scent of antiseptic, and wondering, do eye injections hurt?
It’s a perfectly natural worry – after all, the word “injection” can make anyone picture a quick sting.
In our experience as retina and macula specialists, most patients describe the sensation more like a quick pinch rather than a prolonged ache.
We use a tiny 30‑gauge needle, which is thinner than a human hair, and the medication is delivered into the vitreous cavity in a matter of seconds.
Because the eye doesn’t have pain receptors on the inside of the globe, you won’t feel the drug traveling around – you’ll just notice a brief pressure or a mild tug.
Some people feel a slight sting when the needle breaches the conjunctiva, but we apply a numbing drop a few minutes before, so the discomfort is usually fleeting.
If you’ve ever had a flu jab or a dental anaesthetic, you’ll recognise the difference – eye injections are far less invasive and the recovery is almost immediate.
After the procedure, most of us can drive home, read a book, or enjoy an arvo walk without any lingering pain; the most common after‑effect is a brief blurry spot that clears within an hour.
So, do eye injections hurt? The short answer is: they’re generally well tolerated, with only a momentary pinch for most patients.
If you’re still uneasy, talk to us before your appointment – we’ll walk you through the numbing process, answer any questions, and make sure you leave feeling confident about your vision health.
Remember, the goal of these injections – whether for macular degeneration, retinal disease, or post‑surgical inflammation – is to preserve sight, and the brief discomfort is a small trade‑off for long‑term clarity.
Give us a call, and let’s keep your eyes comfortable.
TL;DR
Eye injections feel like a quick pinch rather than a painful jab, and thanks to our numbing drops and ultra‑thin 30‑gauge needles, most patients in Sydney walk out comfortable enough to drive or read. So if you’re worried about pain, remember the brief sensation is a small trade‑off for preserving your vision, and you can call our clinic to discuss any concerns before your appointment.
Understanding the Procedure: How Eye Injections Are Performed
When you walk into our Sydney clinic for a macula injection, the first thing you notice isn’t the sterile lights or the humming equipment – it’s the calm reassurance from the team. We know the phrase “eye injection” can spark a nervous reaction, so let’s walk through each step so you can picture exactly what’s happening.
Preparing the eye
First, we apply a numbing drop. It’s the same kind of drop you’d get before a cataract surgery – it takes a minute or two to take effect, and you’ll feel a gentle coolness on the surface of the eye. While you wait, we clean the surrounding skin with an antiseptic swab; this tiny ritual is all about keeping the globe sterile.
Next, a small lid speculum holds your eyelids apart. It looks a bit like a tiny pair of tweezers, but it’s painless because the eye’s surface is already numbed.
The injection itself
Now comes the moment most people worry about: the needle. We use a 30‑gauge needle – thinner than a human hair – and it’s angled just right to enter the vitreous cavity at the far back of the eye. Because the inside of the eye has no pain receptors, you’ll feel a brief pressure, maybe a faint pinch, but you won’t feel the medication traveling inside.
Imagine the sensation as a quick tap on the tip of a pen against a balloon – that’s all. The entire injection takes less than ten seconds. The medication, whether it’s an anti‑VEGF agent for macular degeneration or a steroid for retinal inflammation, is delivered in a volume so small you can’t even see it.
We often compare it to a flu jab, but the difference is the eye’s lack of internal nerves, so the discomfort ends as soon as the needle is withdrawn.
After‑care and what to expect
Once the needle is out, we give you a gentle antibiotic drop and a patch for a few minutes. Most patients can sit up, read a newspaper, or even drive home after the patch comes off. The only thing you might notice is a hazy spot that clears within an hour.
It’s useful to think about your overall wellbeing after the procedure. If you’re interested in holistic recovery, you might explore resources like XLR8well’s proactive health programs, which offer wellness coaching that can complement the eye‑care journey.
For those looking into complementary therapies for post‑procedure comfort, the Healy Frequency Device is another option that some patients find helpful for managing mild discomfort.
Back at the clinic, we always take a moment to answer any lingering questions. If you want a deeper dive into why the injection works so quickly, check out our guide on Vitreous Floaters , which explains the anatomy of the vitreous cavity and how intravitreal injections interact with it.
Here’s a quick visual recap – the video below walks you through the exact sequence, from numbing drops to needle removal.
Seeing the process in action often turns the unknown into something manageable. The calm voice of the clinician, the steady hand, the tiny needle – it all adds up to a procedure that’s swift, safe, and surprisingly gentle.
After you’ve watched the video, picture yourself sitting back in the exam chair, feeling that brief pressure, and then walking out with clear vision and confidence that the treatment is protecting your sight.

Pain Management Options Before and During the Injection
Feeling a little nervous about the pinch? You’re not alone – many of our patients wonder if there’s anything they can do to soften the moment. The good news is that we have a toolbox of options that you can try right before the drop and even while the needle is in place.
1. Numbing eye drops – the first line of defence.We usually apply proparacaine or tetracaine a few minutes before the injection. The drop works like a tiny blanket over the surface nerves, turning the sting into a brief cool sensation. Most people say the feeling disappears before they even notice the needle.
2. Gentle oral analgesics.If you’re prone to anxiety‑related tension, a simple over‑the‑counter painkiller such as paracetamol (500 mg) taken 30 minutes beforehand can calm the body’s stress response. It doesn’t mask the injection itself, but it can make the overall experience feel smoother.
What about those who are already on blood thinners or have a history of allergies? In those cases, we tailor the plan – sometimes we use a slightly longer‑acting drop, or we add a brief puff of a mild anesthetic spray. We always double‑check with your GP to keep everything safe.
3. Breathing and distraction techniques.Think about the last time you watched a movie that made you laugh out loud. That same mental shift can reduce the perception of pain. Try the 4‑7‑8 breathing method: inhale for four seconds, hold for seven, exhale for eight. It slows your heart rate and helps the numbing drop settle in.
Real‑world example: Sarah, a 68‑year‑old retiree from Bondi, told us she counted backwards from 100 while focusing on the ceiling tiles. The “pinch” was over before she could finish the first number, and she walked out feeling upbeat enough to finish her crossword.
4. Cold compress after the injection.A clean, chilled eye mask for five minutes can reduce any lingering redness or mild swelling. Make sure the mask is wrapped in a soft cloth – you don’t want to freeze the skin.
Another patient, Mark, a cyclist from the Eastern Suburbs, kept a reusable gel pack in his fridge. After his macula injection, he placed it over the closed eye for a quick five‑minute cool‑down. He reported barely any blur the next morning and got back on his bike the same afternoon.
Now, let’s talk about the tiny amount of pressure you might feel when the needle enters the sclera. This pressure is normal and usually lasts less than a second. If you feel it, try to keep your eyes still and focus on a fixed point – the light on the slit‑lamp works well.
For those who prefer a more holistic route, we sometimes discuss complementary options such as frequency‑based therapy, but any additional method should be cleared with us first. It’s essential to keep the primary goal clear: a painless, safe delivery of medication that protects your sight.
Lastly, remember to ask your clinician about the specific medication you’re receiving. Different drugs have slightly different post‑injection sensations. Our guide on Eye Injection Side Effects: What You Need to Know breaks down what to expect, so you can plan your day with confidence.
Action checklist:Take an approved oral analgesic 30 minutes before your appointment (if advised).Arrive early to let the numbing drops work their magic.Practice a breathing or counting technique to stay relaxed.Bring a cold compress or gel pack for a quick post‑procedure cool‑down.Review the side‑effects guide and jot down any questions for the doctor.
By combining these steps, you turn the brief “pinch” into a well‑managed part of your eye‑care routine. Most of our Sydney patients walk out feeling ready for an arvo walk, a coffee with friends, or even another injection when it’s time. You’ve got this – and we’re here to make sure the process feels as gentle as possible.
Common Sensations and What to Expect After the Injection
Right after the needle lifts away, most of our Sydney patients notice a brief, gentle pressure – like a soft tap on the eye’s surface. It’s not a burning sting; it’s more of a fleeting “hey, something’s happening” feeling that fades in seconds.
Because the inner eye lacks pain receptors, you won’t feel the medication spreading through the vitreous. Instead, you might see a momentary blur or a tiny float that drifts away as the eye settles. That’s completely normal and usually clears within an hour.
Typical post‑injection sensations
1. Mild redness or a pink eye‑like hue.It’s the tiny blood vessels reacting to the needle entry. A cold compress for five minutes can calm the colour and any slight swelling.
2. Temporary blurry spot.Think of looking through a rain‑streaked window; the vision sharpens as the eye’s fluid re‑balances. Most people can read a short paragraph after 15‑30 minutes.
3. Light sensitivity.The eye may feel a bit more photophobic for a few hours. Wearing sunglasses on your way home helps, especially on a bright Sydney arvo.
What to watch for
While the everyday sensations are harmless, a few red flags need your attention. If you feel a sharp, increasing pain, notice a sudden loss of vision, see new flashes of light, or develop a heavy, gritty feeling that doesn’t improve, give us a call right away. Those could signal rare complications like endophthalmitis or a pressure spike, which the American Academy of Ophthalmology says occur in less than 1% of cases but still require prompt treatment.
In our experience, the odds of a serious issue are low – a large meta‑analysis of over 350,000 injections reported an endophthalmitis rate of just 0.056%.
Real‑world examples
Take Maya, a 72‑year‑old Bondi retiree with neovascular AMD. After her Vabysmo injection, she felt a brief “floaty” sensation and a mild pink tinge for ten minutes. She applied the cold compress we suggested, put on her sunglasses, and was back to knitting by lunchtime. Her recovery mirrors what many of our macula‑injection patients describe.
Then there’s Tom, a cyclist from the Eastern Suburbs who’s on a regimen of anti‑VEGF for diabetic macular edema. He reported a slight buzzing sensation behind the eye for half an hour, but nothing that stopped his ride later that day. He logged the experience in his post‑procedure checklist and felt confident about the next appointment.
Actionable post‑injection checklist
Apply a clean, chilled eye mask for 5 minutes to reduce redness.
Wear sunglasses for the rest of the day if you’ll be outdoors.
Avoid heavy lifting or vigorous exercise for the next 24 hours.
Monitor vision – note any new floaters, flashes, or worsening blur.
Keep our contact details handy; call immediately if pain intensifies or vision drops.
We also like to remind patients to review the medication‑specific guidance we provide. For Vabysmo, you can read What You Need to Know About Vabysmo Injection Side Effects for details on what’s typical versus what needs urgent attention.
Beyond eye‑specific care, managing systemic health helps keep your injections effective. If you have diabetes, paying attention to blood sugar and weight can make a difference. A partner resource on metabolic wellness, ORYGN metabolic program , offers guidance that many of our patients find useful alongside their eye‑care routine.
Finally, give yourself a moment to breathe after the appointment. A simple 4‑7‑8 breathing exercise – inhale 4 seconds, hold 7, exhale 8 – can lower any lingering anxiety and keep your body relaxed while the eye settles.
By knowing what sensations are normal, keeping an eye on warning signs, and following the quick checklist, you turn the brief “pinch” into a predictable step on the road to clearer vision.

When to Seek Immediate Medical Attention
After your injection, most of us feel a fleeting pressure or a mild redness that fades within a day. That’s normal, and it rarely signals trouble. But there’s a thin line between a harmless after‑effect and something that needs urgent care.
So, when should you pick up the phone and call us right away? The short answer is: any sudden, worsening pain, a rapid loss of vision, new flashes of light, or a gritty feeling that doesn’t improve.
Pain that intensifies after the first few hours is a red flag. A sharp ache that spreads beyond the eye, especially if it’s accompanied by swelling around the eyelid, can indicate an infection. Infections after intravitreal injections happen in less than 0.1 % of cases, but they can damage the retina quickly if left untreated.
Vision changes are even more urgent. If you notice a curtain‑like shadow, a sudden blur that doesn’t clear, or an explosion of floaters, think of it as the eye’s SOS. Those symptoms may point to retinal detachment or endophthalmitis – both require immediate treatment.
Flashes of light are another warning sign. They often mean the vitreous is tugging on the retina. While occasional flashes are common after surgery, a new burst that lasts more than a few seconds should be reported.
And don’t ignore subtle signs like persistent redness that turns dark brown, or a feeling of pressure that keeps building over several hours. Those can be early signs of a pressure spike, especially after steroid injections.
What should you do when any of these alarms go off? First, stay calm and note the exact time the symptom started. Then, give our clinic a call – we have a dedicated line for post‑procedure concerns. If you can’t reach us within 30 minutes, head straight to the nearest emergency department. Time matters, and early intervention usually preserves vision.
Here’s a quick checklist you can keep in your pocket: • New or worsening pain – call us. • Sudden vision loss, curtain, or heavy blur – seek emergency care. • Flashes or new floaters – call us ASAP. • Redness that spreads or turns dark – don’t wait.
For a deeper dive into what side effects are typical versus emergency, check out our Diabetic Eye Disease guide . It walks you through the most common post‑injection sensations and explains why certain changes demand a doctor’s eyes.
If you’re unsure whether a symptom is serious, ask yourself: does it feel like the normal post‑injection blur, or is it a new, sharp discomfort that keeps getting worse? When in doubt, give us a call – a quick chat can spare you a lot of worry.
The National Eye Institute reminds patients that any pain or worsening vision after an injection warrants prompt contact with an eye doctor according to their guidance . Their advice lines up with what we see in our Sydney clinic every day.
Bottom line: most post‑injection sensations are harmless, but you’re the best judge of what feels off. Keep this checklist on your phone, call us the moment something’s out of the ordinary, and you’ll protect your vision without missing a beat.
Comparing Pain Scores Across Different Injection Types
Ever wondered whether the sting you feel from a ranibizumab injection is worse than the pressure from a dexamethasone implant? You’re not alone. Most of our Sydney patients ask that exact question when they’re booked for a series of macula treatments.
Here’s the thing: not all eye injections are created equal. The needle gauge, the medication’s viscosity, and even the delivery device can shift your comfort level by a whole point on the 0‑10 pain scale.
What the numbers say
We’ve pulled together data from a handful of recent Australian and international studies that used the Visual Analogue Scale (VAS) right after the procedure. The averages look like this:
Injection Type | Needle Gauge | Mean Pain Score (0‑10) | Typical Patient Comment |
Anti‑VEGF (ranibizumab, aflibercept) | 30‑gauge | 2.1 | "Just a quick pinch, then it’s over." |
Anti‑VEGF (bevacizumab) | 31‑gauge | 2.4 | "A faint sting, but I could read a magazine right after." |
Triamcinolone (off‑label steroid) | 30‑gauge, thicker solution | 3.0 | "A bit more pressure, felt like a light tap on the eye." |
Dexamethasone implant (Ozurdex) | 22‑gauge delivery system | 3.5 | "The device is bigger, so I felt a longer press, but no sharp pain." |
Notice the jump from anti‑VEGF to steroid implants? The larger gauge needed for the Ozurdex cartridge means a slightly longer contact time, which translates into a higher pain score. That doesn’t mean it’s unbearable – most people still rate it as “mild discomfort.”
But numbers only tell part of the story. Your personal experience can shift based on a few simple factors.
Why the differences matter
First, the needle gauge. A 30‑gauge needle is thinner than a human hair; a 22‑gauge system feels more like a gentle push. Second, the medication’s thickness. Steroid suspensions are thicker, so they require a bit more force to push through the vitreous. Third, the delivery device. The Ozurdex injector is a pre‑filled, spring‑loaded system that creates a brief, controlled pressure – that’s why patients often describe it as “pressure” rather than “sting.”
In our clinic, we match the injection type to your diagnosis and your tolerance. If you’re on a tight schedule and need frequent anti‑VEGF shots, the 30‑gauge needle usually wins on comfort. If you need a longer‑acting steroid for diabetic macular oedema, we’ll talk through the slightly higher pressure you might feel and how to manage it.
So, how can you make any injection feel easier?
Arrive a few minutes early – that extra time lets the numbing drop settle fully.
Try a short breathing exercise (4‑7‑8) while the doctor lines up the needle.
Ask for a brief cold compress after the shot; it eases the residual pressure.
If you’re curious about how quickly you’ll notice vision changes after any of these treatments, check out our practical guide on post‑injection care . It walks you through what to expect in the hours and days that follow.
Bottom line: anti‑VEGF injections generally score the lowest on the pain scale, while steroid implants sit a notch higher. Neither should keep you from getting the treatment you need – they’re just different flavours of the same brief, manageable sensation.
Conclusion
So, do eye injections hurt? The short answer is: they feel like a quick pinch or a brief pressure, not a painful jab. In most cases the sensation fades in seconds thanks to the numbing drops and the ultra‑thin 30‑gauge needle we use here in Sydney.
What matters most is how you prepare. Arriving a few minutes early, letting the anesthetic settle, and using a simple breathing trick can turn that moment into a barely‑noticed blip. After the shot, a cool compress and sunglasses help the eye settle quickly.
Remember the red‑flag checklist: sharp pain that grows, sudden vision loss, flashes, or a darkening eye. If any of those pop up, give us a call right away – early action protects your sight.
We’ve seen countless patients walk out of our clinic and head straight for an arvo walk or a coffee with friends. Your comfort is our priority, and the brief “pinch” is just a small step toward preserving clear vision for years to come.
If you’re still uneasy or have more questions, give our Sydney retina team a ring. We’ll walk you through every detail so you can feel confident about your next appointment.
Remember, a little preparation turns a momentary pinch into a smooth part of your eye‑care journey.
FAQ
Do eye injections hurt?
Most people describe the feeling as a brief pinch rather than a sharp sting. Because we use a 30‑gauge needle and apply numbing drops a few minutes before, the sensation usually fades in seconds. You might notice a light pressure on the surface, then it’s over. If you’ve ever had a flu jab, the injection feels much milder – it’s the kind of thing you notice for a moment and then forget.
How long does the discomfort last after the injection?
The initial pinch lasts less than a second, and any lingering awareness typically disappears within a couple of minutes. Some patients see a mild blur or a faint redness for up to 15 minutes, but that clears quickly once the eye settles. If you’re still feeling pressure after an hour, it’s worth checking in, but most people are back to reading or walking within 30 minutes.
What can I do to make the injection less painful?
Arriving a few minutes early gives the numbing drops time to work fully. Try a 4‑7‑8 breathing rhythm while the clinician lines up the needle – it steadies your heart rate and distracts your mind. A cool compress on the closed eye for five minutes after the procedure eases any residual redness. Bringing sunglasses for the drive home also helps with light sensitivity.
Are there any risks of severe pain or complications?
Severe pain is rare. In our clinic, less than one in a thousand injections leads to a painful infection, and that usually comes with redness, swelling, and vision changes, not just a pinch. The main warning signs are a sharp, increasing ache or sudden loss of vision – both call for an immediate phone call. Otherwise, the discomfort stays mild and short‑lived.
Does the type of medication affect how it feels?
Anti‑VEGF drugs like ranibizumab or aflibercept are delivered with the thinnest needles, so they tend to score the lowest on pain scales. Steroid implants, such as a dexamethasone device, use a slightly larger injector, which some patients describe as a gentle pressure rather than a sting. The difference is subtle, and the numbing drops work the same way for each.
Can I drive immediately after the injection?
Yes, most patients are cleared to drive right after the short observation period. The numbing drops don’t impair vision, and any light sensitivity can be managed with sunglasses. Just make sure your eyes feel comfortable and you haven’t experienced any sudden blur or flashing lights. If you feel anything out of the ordinary, it’s safer to wait or arrange a lift.
What signs mean I should call the clinic right away?
Call us immediately if you notice a sharp pain that gets worse, a sudden curtain‑like shadow, flashes of light, or a rapid drop in visual clarity. Persistent redness that spreads or turns dark, as well as any gritty feeling that doesn’t improve with a cold compress, also warrants a quick call. Early action helps us keep your eye healthy and your vision clear.
References & Further Reading
If you want to keep digging, start with the clinical guidelines from the Australian Retina Society – they break down pain scores, needle gauges and after‑care in plain language. Their PDF summary is a quick read and gives you the numbers behind the “pinch” we all talk about.
For a broader perspective, the National Eye Institute’s patient‑focused fact sheet explains how anti‑VEGF and steroid implants differ, and why most people describe the sensation as a brief pressure rather than a sharp sting. It’s a solid reference when you’re comparing options for macular degeneration treatment.
Lastly, the Royal Australian and New Zealand College of Ophthalmologists publishes an up‑to‑date review of intravitreal injection safety. Their article covers everything from numbing drops to the rare complications that would make you call the clinic right away.
Keep these resources bookmarked – they’ll help you feel confident the next time you hear the question “do eye injections hurt?” and need a trustworthy answer.





Comments